What Is a Speech Language Pathologist & What Do They Do?
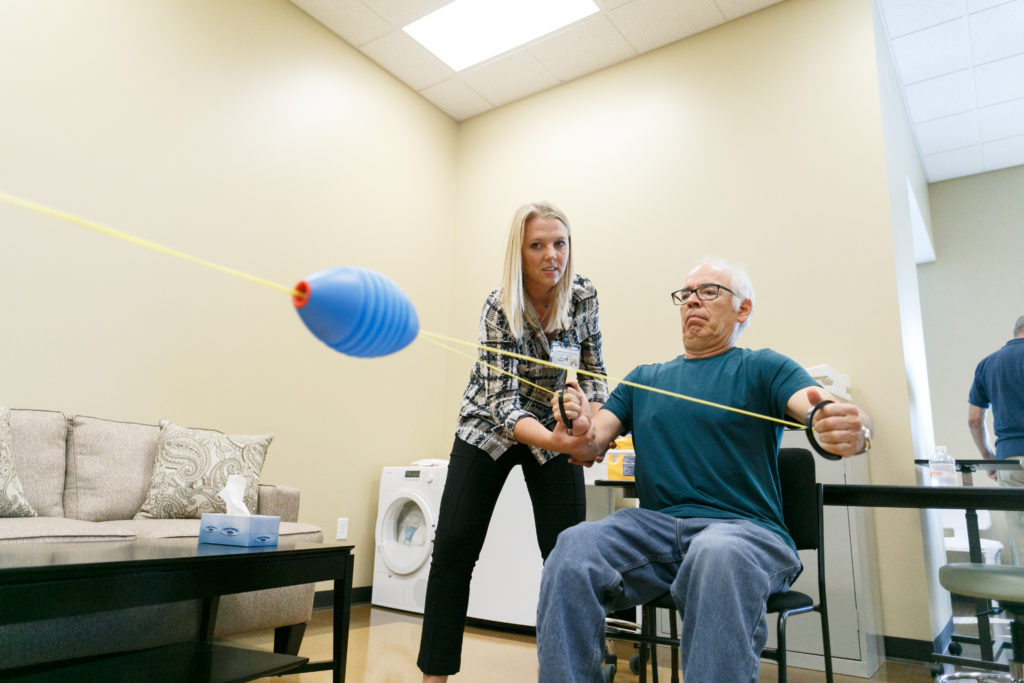
A speech-language pathologist (SLP) diagnoses and treats issues related to speech, language, communication and swallowing disorders.1 For patients struggling to communicate or swallow, these healthcare professionals help them to better engage with the world around them. Read on to learn more about this exciting and promising career. Table of Contents: What Do Speech-Language Pathologists Do?