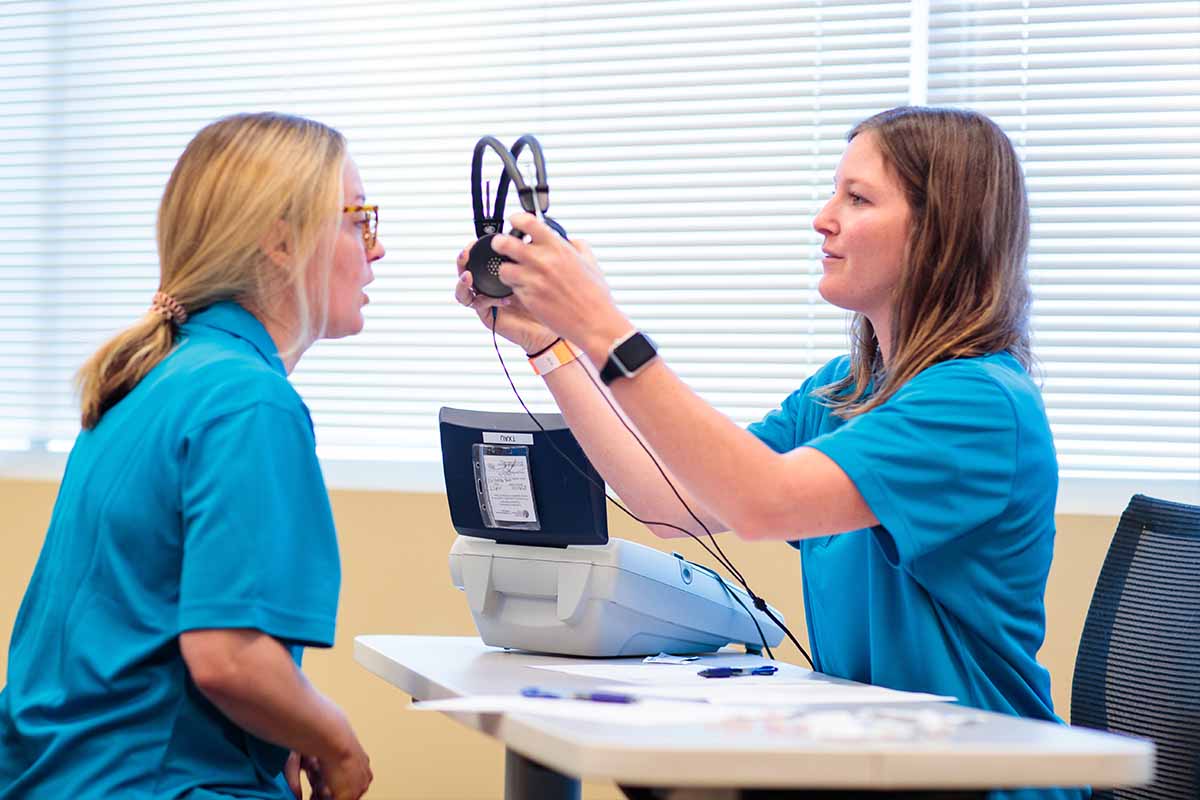
Fourth-term speech-language pathology (SLP) students on the University of St. Augustine for Health Sciences (USAHS) Austin campus are learning through interprofessional simulation scenarios, practicing patient interactions with their peers in our physical therapy (PT) and occupational therapy (OT) programs. In our state-of-the-art Center for Innovative Clinical Practice (CICP), students engage in complex scenarios, learning how to communicate with each other and treat the patient as part of a team.
“Today’s health professionals need to work together to create better patient outcomes,” says Kathy Wheat, PhD, CCC-SLP, founding program director of the university’s MS-SLP program. “An inability to work together will negatively impact patient care. We are prioritizing interprofessional education so our students are ready to prioritize interprofessional collaboration on the job.”
One of our DPT students weighed in: “I found this [lab] very beneficial because I have little to no experience working with OTs or SLPs. Not only did I learn more about what OTs and SLPs do, but also how the three healthcare professions can work together in order to achieve patient/family goals.”
Practice patient interactions in interprofessional teams with PTs, OTs


How It Works
To create the scenarios, SLP faculty members draw on their own clinical experience and solicit input from OT and PT faculty. Each scenario maps to one of the four core competencies identified by the Interprofessional Education Collaborative (IPEC): values and ethics, roles and responsibilities, interprofessional communication, and teams and teamwork.
The students act out the scenario with a faculty member or student playing the mock patient. All role-plays are videotaped for later playback. Students use the PEARLS (Promoting Excellence and Reflective Learning in Simulation) debriefing tool to discuss how they responded, what they did well, and what they could do differently for a better patient outcome and to lower healthcare costs.
Different Types of Scenarios Each Term
Associate Professor Meghan Savage, PhD, CCC-SLP, leads the simulations along with OT and PT faculty members. Dr. Savage says that during Trimesters 1 and 2, the scenarios focus on professionals introducing themselves and their scope of practice to the patient, parent, and caregiver. Trimester 3 scenarios are about ethics and teamwork. Examples of scenarios include:
- A parent who doesn’t ask a lot of questions, just sitting there taking in information, versus a parent who is very vocal. Team members practice communicating with the parent and each other.
- A child with cerebral palsy who can communicate basic needs but needs an AAC (augmentative and alternative communication) device for more complicated communication. Team members identify areas of speech, mobility, and function they can address.
- An older woman who lives in a second-floor apartment with her daughter and grandchildren. She typically watches the grandchildren while her daughter is at work. Following a stroke, she is gets discharged from the hospital and has speech, swallowing, and mobility issues. Will she be able to watch the kids?
During trimesters four and five, the skills will be based on describing patient assessments and treatments. For example, for a patient with Parkinson’s disease, professionals have different goals:
- The SLP has goals related to swallowing, voice, and cognition.
- The OT has goals related to orientation, cognition, daily living skills, mental health, and adaptive equipment.
- The PT has goals related to gait and mobility.
Student Feedback
Dr. Savage says the feedback from students has been very positive. “It’s exciting to watch students explore other disciplines. We can see the light bulb go off. The PTs and OTs say, ‘I didn’t realize that SLPs work with swallowing and cognition as well as with language.’ SLP students say, ‘I didn’t realize that OTs work with social skills and cognition.’ Students learn the value of teamwork and have called us ‘our own cool gang of rehab professionals!’”
SLPs can teach PTs how to communicate with a child who has a language delay or disorder; or they can work with the child on speech issues while the PT works on walking. For a patient who has mobility and swallowing issues following a stroke, the PT can help position the patient, the OT can help with the fine motor skills of eating, and the SLP can work on swallowing. Students can learn these skills in a safe environment in clinical simulation. The goal is for students to learn and appreciate how to implement interprofessional collaborative practice to help improve client outcomes and ultimately reduce healthcare costs. “I wish I’d had this chance in graduate school!” Dr. Savage says.
The program also features SLPs-only skills-based simulations in the hospital ward of the CICP. Under the guidance of instructors, students practice conducting bedside swallow, oral mechanism, and cranial nerve exams. Students can count up to 75 sim lab hours toward the 400 clinical externship hours required for CCC-SLP certification by the American Speech-Language-Hearing Association (ASHA).
“Before interprofessional education, working together was a matter of trial and error,” says Dr. Wheat. “Now students can practice this so they are ready for their career.”
The University of St. Augustine for Health Sciences (USAHS) offers a Master of Science in Speech-Language Pathology (MS-SLP). Designed for working students, the MS-SLP is an online program with four required on-campus residencies on the USAHS Austin campus. Prepare to make a difference in the lives of clients across the lifespan with a meaningful career in speech therapy!
For students with a bachelor’s degree in a field other than communications sciences and disorders (CSD) or SLP, we offer SLP leveling courses for completing the necessary pre-requisites to enter the graduate program.