In a pro bono clinic based at our physical therapy school in Miami, USAHS students are helping people with Parkinson’s disease improve their balance, coordination, and quality of life. Guided by faculty, Doctor of Physical Therapy students plan and lead virtual classes in Rock Steady Boxing, a non-contact, boxing-based fitness curriculum.
“Rock Steady Boxing helps people with Parkinson’s because it involves aerobic exercise, rotational movements, and power generation,” says assistant professor Miguel Garcia, PT, DPT, EdD, who spearheaded this initiative.
“The mixture of movements and high-intensity exercise, when combined with the appropriate medication management, has been shown to help slow the disease process.”
In early 2020, Dr. Garcia trained to be a Rock Steady Boxing coach with the plan to create a program on campus. He would bring in patients from the Brain Center, an outpatient neurological clinic in Miami with which he had a longstanding relationship. A nonprofit organization, the Brain Center offers free community programs for people with neurological issues, such as Parkinson’s, multiple sclerosis, and dementia.
Dr. Garcia and his colleagues in the Miami DPT program—interim program director Dr. Gabriel Somarriba, Dr. Tatiana Godoy Bobbio, and Dr. Caprice Quiñones—collaborated to design an in-person boxing class and integrate it into Neuromuscular II, a core course for DPT students in their sixth trimester.
But before the classes could begin, the COVID-19 pandemic upended plans to host them on campus. Faculty decided to move forward—in a virtual mode. The weekly Zoom classes began in Fall 2020 and are ongoing today. “Each class consists of an active warm-up, followed by strengthening and functional mobility exercises,” Dr. Garcia says. “The boxers are getting a good exercise class, and the students are learning how to communicate and work with patients. This isn’t simulation—it’s real people.”
How Classes Work
At the beginning of Neuromuscular II, students read research studies about the effects of Parkinson’s on the brain and how PT treatment approaches can help. Faculty members lead the first Rock Steady Boxing class; the students work together in small groups, with guidance from faculty, to develop all subsequent classes. “They mimic what they’ve seen and add their own ideas,” says Dr. Garcia. “Some students have a boxing background, which is fun.”


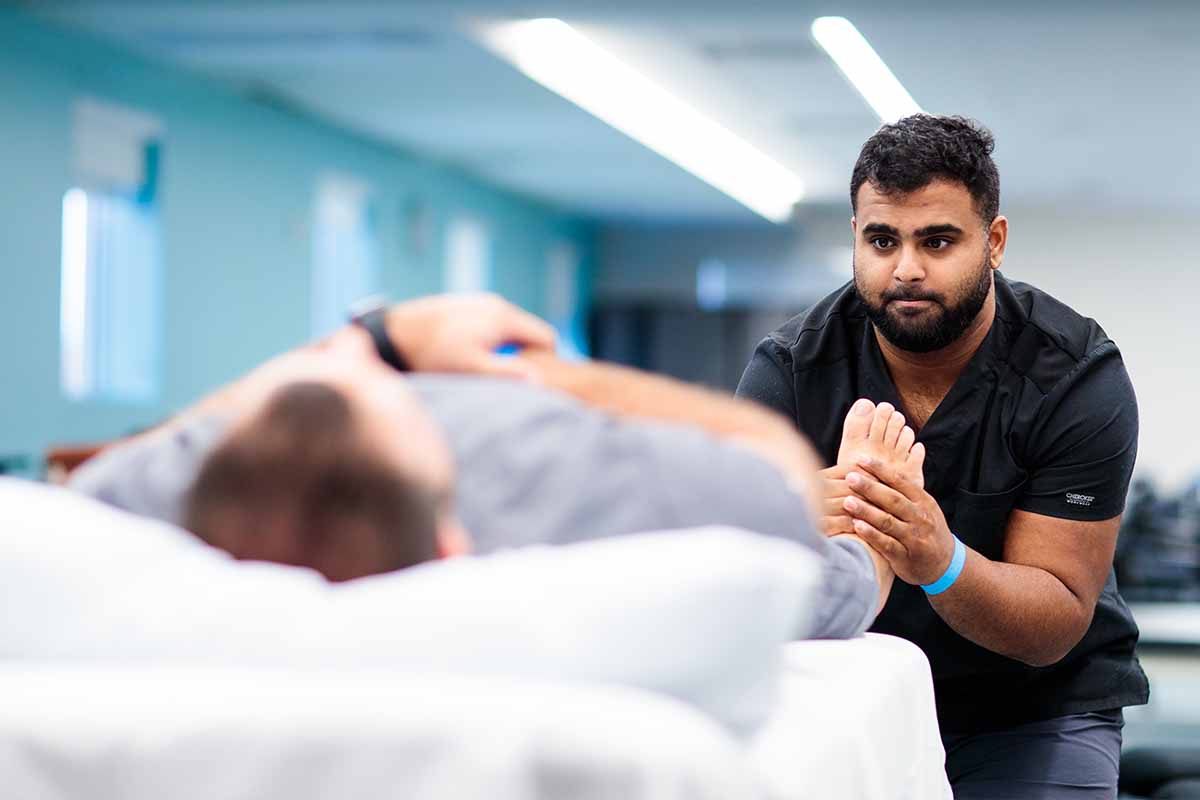
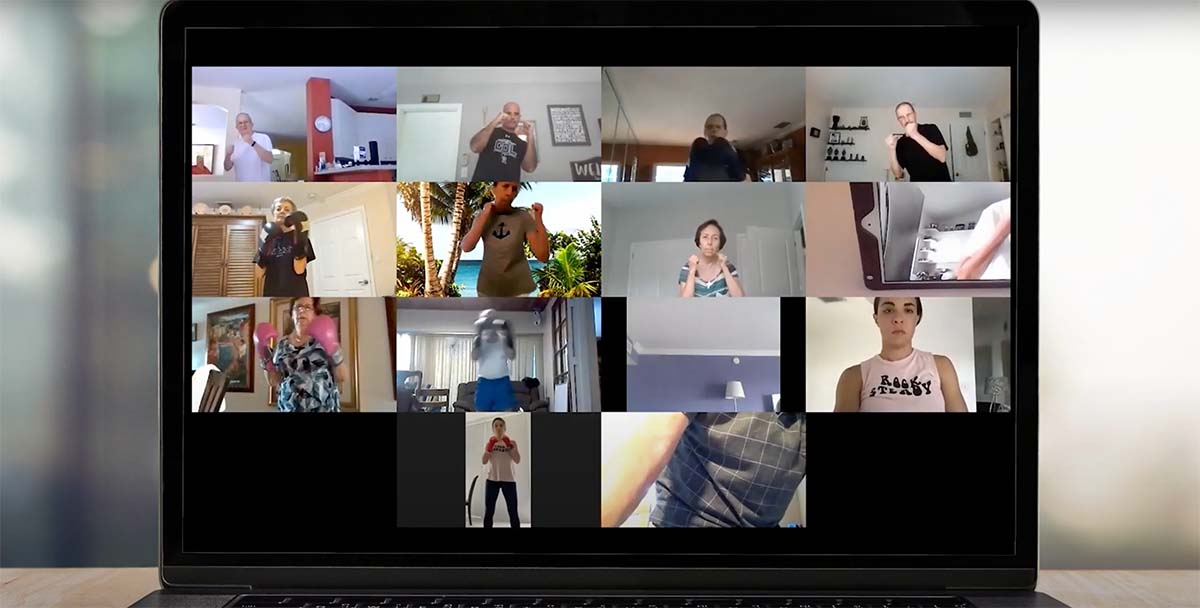
Two students and Dr. Garcia (right) teach a Rock Steady Boxing class. RIGHT: Boxers join the class on Zoom.
He explains that the participants, or “boxers,” have a wide range of functional capacity. Some must sit in a chair due to the disease progression, while others have a nearly invisible level of impairment. Some boxers simply shadowbox, while others use equipment that would be present in an in-person class, such as boxing gloves, punching bags, and weights. Or for resistance, they can use objects like water bottles and cans of soup.
“The students love it,” says Dr. Garcia. “It’s great to see how excited they are to work with real patients. They’re humbled by how much they can push the boxers and challenge their cardiovascular systems.” He explains that the latest evidence-based research has demonstrated the benefits of reaching a moderate to high level of intensity within treatment. “The boxers only rest for about five minutes during the whole hour,” he says.
“They love that they’re not being treated as fragile. They are interactive with the students. Most have been doing Rock Steady Boxing for a while, even before our class, so they can guide the students and tell them to increase or lower the intensity.”
Of course, boxers can take breaks whenever they need to.
When asked what he gets out of this program, Dr. Garcia is effusive. “For me it’s fantastic. It’s a taste of the clinic in the classroom. It’s what made me fall in love with the profession in the first place. And the patients get better—I see how it’s affected their lives in a positive way.”
On-campus boxing classes are slated to begin in the Summer 2022 trimester, complete with equipment (gloves, punching bags, and weights).
Dr. Garcia and his three colleagues are currently running a first-of-its-kind research study on the effectiveness of conducting Rock Steady Boxing classes through a telehealth medium. The yearlong study involves 13 participants who respond to questionnaires quarterly about their perception of the classes and their own health outcomes. And once the classes move to in-person, faculty will begin gathering data on the boxers’ changes in cardiac capacity.
A Second Pro Bono Clinic: Fall Prevention
Before he got involved in Rock Steady Boxing, Dr. Garcia traveled to the Netherlands to train in a Dutch falls prevention program that had demonstrated success in reducing patients’ incidence of injury with falls. He partnered with the Brain Center to bring neurological patients (with their doctor’s authorization) to campus for a pro bono clinic focused on falls prevention that began in 2019.


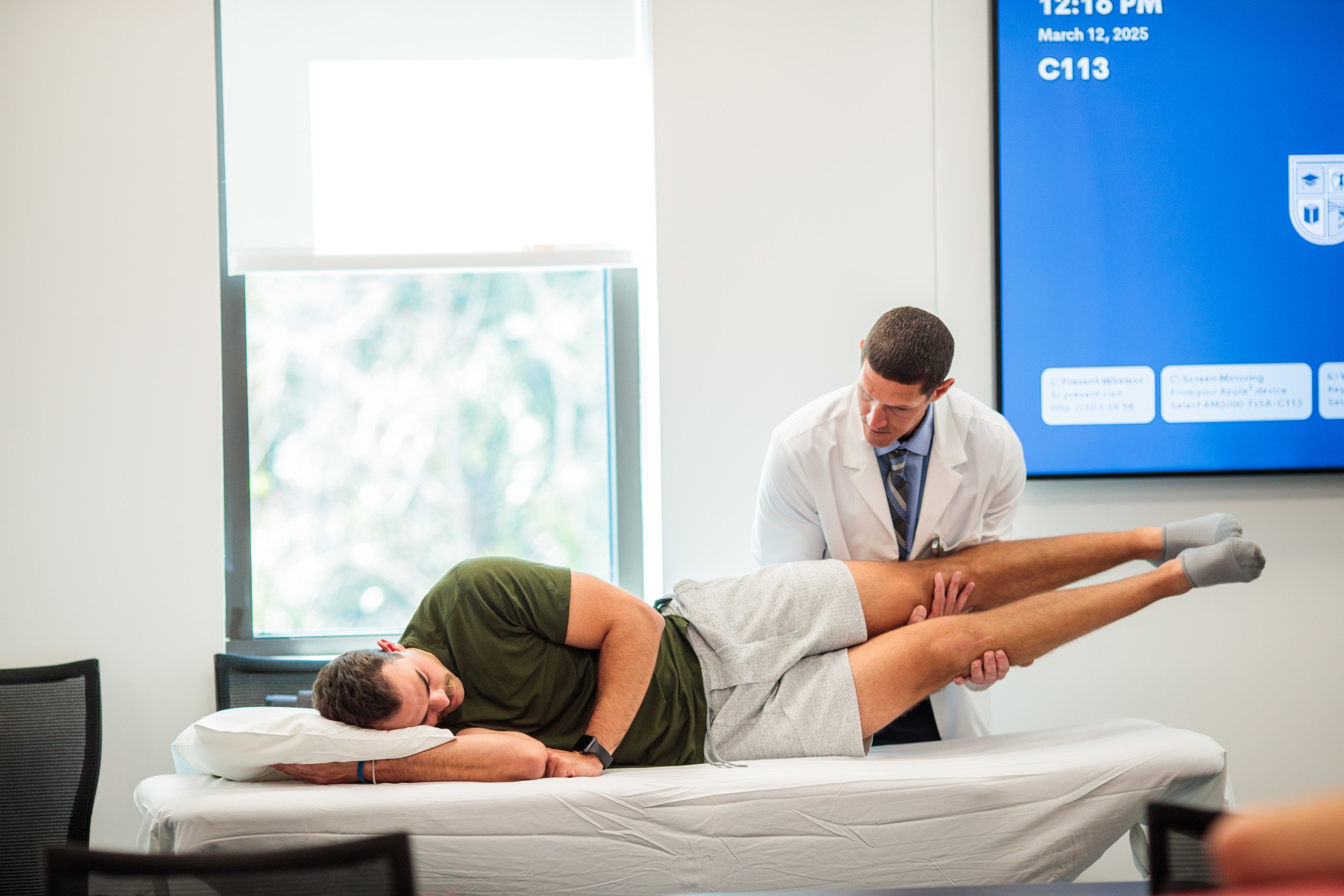
LEFT: Students guide participants to safely navigate the obstacle course. RIGHT: Dr. Garcia (top right) and students teach fall techniques.
Dr. Garcia converted a classroom into an obstacle course, with planks of wood that mimic an uneven sidewalk, stairs, etc. Participants practiced dynamic gait training, throwing and avoiding rubber balls, walking and turning while carrying objects, squatting, and performing judo rolls on high mats. “The highlight of the program is teaching the participants how to safely fall, based on martial arts techniques,” he says. “Each participant works with one or two students at a time, so it is very individualized and safe.”
This clinic ran from Summer 2019 through Spring 2020, when it went to a limited virtual format due to the pandemic. Plans are underway for it to restart in person this March. This program also has a research component; Dr. Garcia is collecting data from participants on whether the number and severity of falls are reduced.
The Benefits of Integrating Patients into the Classroom
Dr. Garcia joined the USAHS faculty in 2009 with a background in clinical practice and leadership. He had previously served as the director of rehabilitation at West Gables Rehabilitation Hospital in Miami. In 2018, he embarked on earning his Doctor of Education (EdD) degree at USAHS, graduating in 2021. His dissertation explored the benefits of integrating patients into the classroom setting. “Alongside the two pro bono clinics, I regularly expose students to patients in the classroom—either by inviting patient visitors to campus or by taking the students to a local rehabilitation hospital where I work,” says Dr. Garcia. For his dissertation, he compared students’ self-reported confidence levels across various patient integration experiences.
“Results showed that integration of patients in the classroom setting improved overall student confidence when completing a neurological examination and treatment.”
For Dr. Garcia, the benefits of these patient integration experiences are twofold. “I’m a clinician and an academic, and I love being able to do both at the same time,” he says. “It fulfills my two greatest passions—helping patients and teaching students. It’s great to see students’ aha moments—and everything they’ve learned clicks for them.”
The largest PT school in the United States,* the University of St. Augustine for Health Sciences (USAHS) offers a hands-on Doctor of Physical Therapy (DPT) degree. Join a collaborative cohort of peers who learn under the mentorship of expert faculty-practitioners. Practice with mock and real patients in our state-of-the-art simulation centers and learn anatomy with our high-tech tools. Prepare for clinical practice with a wide range of patients, as well as for advanced roles in research, practice leadership, and policymaking. Residential (blended didactic courses + in-person labs on weekdays) and Flex (online courses + in-person labs on weekends) formats are available.
*Based on total DPT degrees conferred, as reported by the Integrated Postsecondary Education Data System (IPEDS). Data is captured by IPEDS through interrelated surveys conducted annually by the U.S. Department of Education’s National Center for Education Statistics (NCES). https://nces.ed.gov/ipeds/