Mental illnesses are prevalent in the U.S. and globally. The National Institutes of Health (NIH) reported that over one in five U.S. adults, approximately 59.3 million adults, or 23.1% of the adult population, were living with a mental illness.1 The severity of a mental illness can vary from person to person. Some individuals can perform daily tasks, including work, with mental illness, and some people may qualify for disability due to their mental illness.2
Understanding mental health statistics in the United States helps raise awareness and can inform efforts to better support those in need. Here, we discuss how many people struggle with mental health challenges and how prevalent they are across different populations.
It’s helpful to note the difference between mental health and mental illness. Mental health is how a person functions in daily activities, and mental illness is the collective term for all diagnosable mental disorders.3
Table of Contents:
- What Are the Primary Causes of Mental Illness?
- Mental Health Statistics by Type
- Mental Health Statistics by Age
- Mental Health Statistics by Race
- How Mental Illness Affects Individuals
- How Mental Illness Affects Communities
- The Impact of COVID-19 on Mental Health
- Mental Illness and Criminal Justice System Statistics
- Mental Illness in Rural Communities
- Suicide Statistics
- The United States Needs More Mental Health Workers
Key Findings
Mental illness affects people of all ages, genders and races. The following key findings show what types of mental illness are the most common and who they affect the most.
The following image shows some of the key mental health findings in the United States from a variety of organizations:
What Are the Primary Causes of Mental Illness?
Mental illness can have many contributing factors, and professionals in the psychology field often use the biopsychosocial model to understand its underlying causes.4
To diagnose a patient, the industry standard in the United States is to use the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR).5 While the DSM-5-TR diagnosis helps identify the specific illness, the biopsychosocial model allows mental health professionals to see beyond these labels.
The biopsychosocial model helps professionals understand the cause of mental illness by looking at three factors4:
- Biological: Genetics and family history may be the cause of mental illness. It’s also possible that exposure to alcohol or drugs in the womb was a factor.
- Psychological: Stressful events, like a traumatic experience, in a person’s life can alter their psychology and lead to a mental illness.
- Social: Social factors like a person’s home environment, community, relationships, employment status and more can affect a person’s mental health.
It’s helpful to understand this model because it can lead to better treatment and understanding of a person’s mental illness. For example, a person may have symptoms of anxiety and depression after losing a job, which is treated differently from someone who may be struggling with depression due to biological factors. Short-term mental health issues are referred to as situational rather than clinical.6
However, as we discuss adolescent and adult mental health statistics, note that there’s often no differentiation between situational or clinical mental illness.
Mental Health Statistics by Type
The NIH reports that the most prevalent mental illnesses for adults in the United States are various anxiety disorders.7 In terms of mental health statistics 2025, the prevalence of general mental health concerns among adults has been relatively stable from 2021 to 2025, with around 23% of U.S. adults experiencing any mental illness in 2025.8 Anxiety disorders come in many different forms and can include panic disorder, generalized anxiety disorder, social anxiety disorder, phobias and more.
One of the most common forms of mental illness is major depression.9 In 2021, 21 million adults reported having at least one episode of major depression, which is roughly 8.3 percent of the U.S. adult population.9 They also found that there’s a higher instance of depression in adult women than in men.
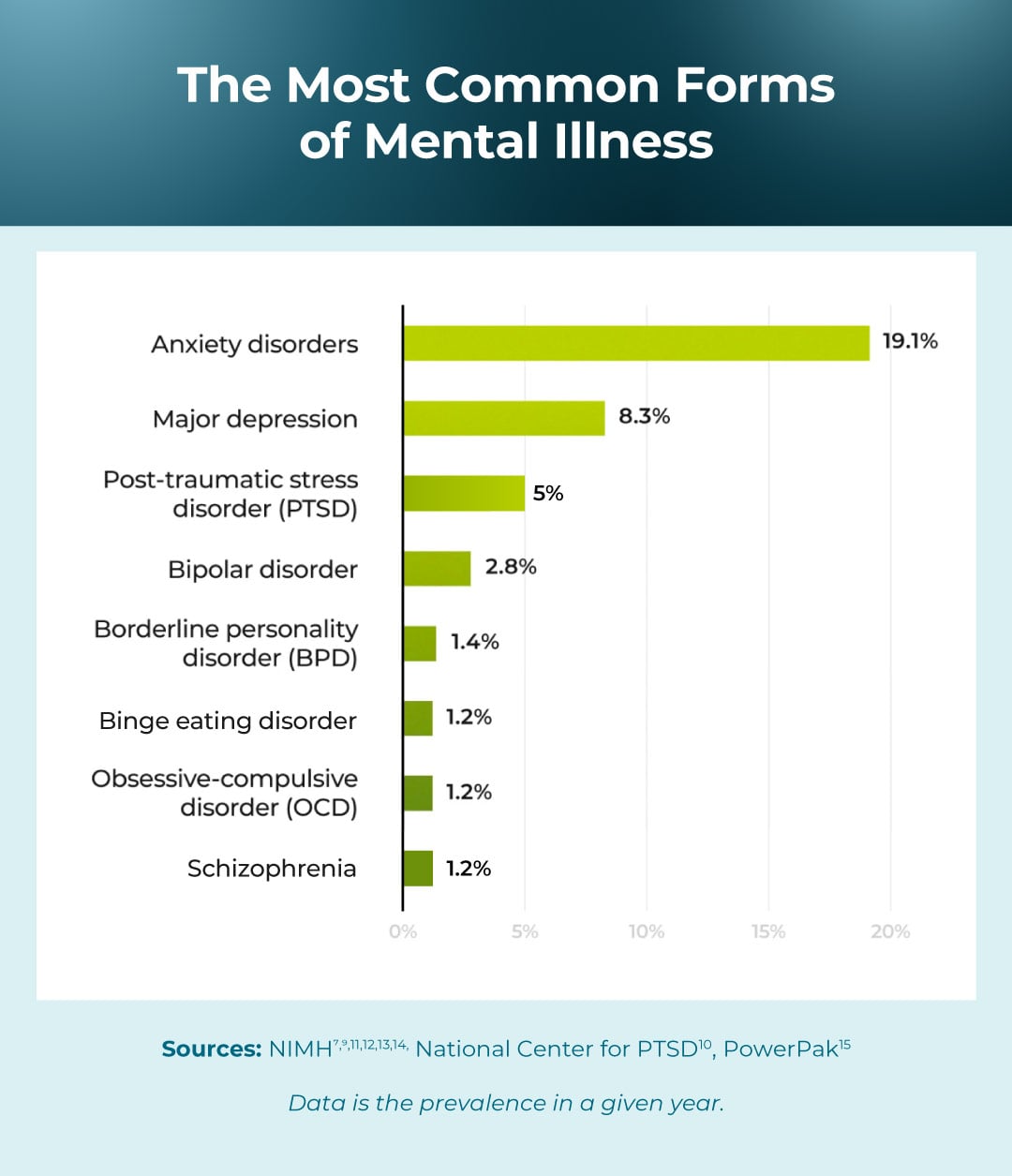
The following are the rates of prevalence of mental illnesses in U.S. adults in a year:
- Anxiety disorders: 19.1%7
- Major depression: 8.3%9
- Post-traumatic stress disorder (PTSD): 5%10
- Bipolar disorder: 2.8%11
- Borderline personality disorder (BPD): 1.4%12
- Binge eating disorder: 1.2%13
- Obsessive-compulsive disorder (OCD): 1.2%14
- Schizophrenia: 1.2%15

Mental Health Statistics by Age
Mental illness can affect anyone, including young people. For those struggling with mental illness, about 50 percent of individuals started to have symptoms by the age of 14, and 75 percent experienced symptoms by age 24.16 Signs can include mood changes, problems thinking, apathy and other unusual symptoms.
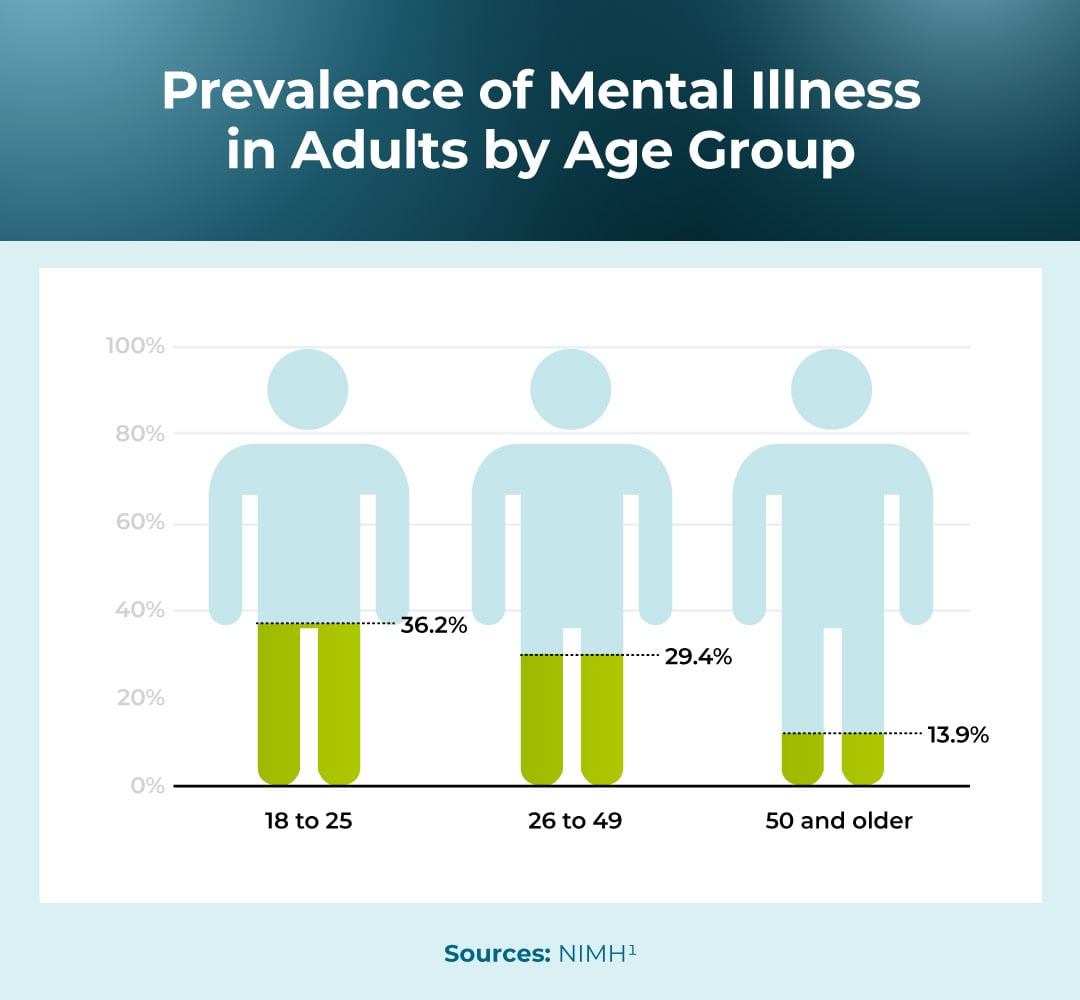
The following is how common mental illness is within different age groups:
There are also millions of adolescents struggling with mental illness:
- The lifetime prevalence of any mental disorder among U.S. adolescents aged 13-18 was shown to be estimated at about 49.5%.1
- Of adolescents with any mental disorder, an estimated 22.2% had severe impairment and/or distress. DSM-IV based criteria were used to determine severity level.1
Mental Health Statistics by Race
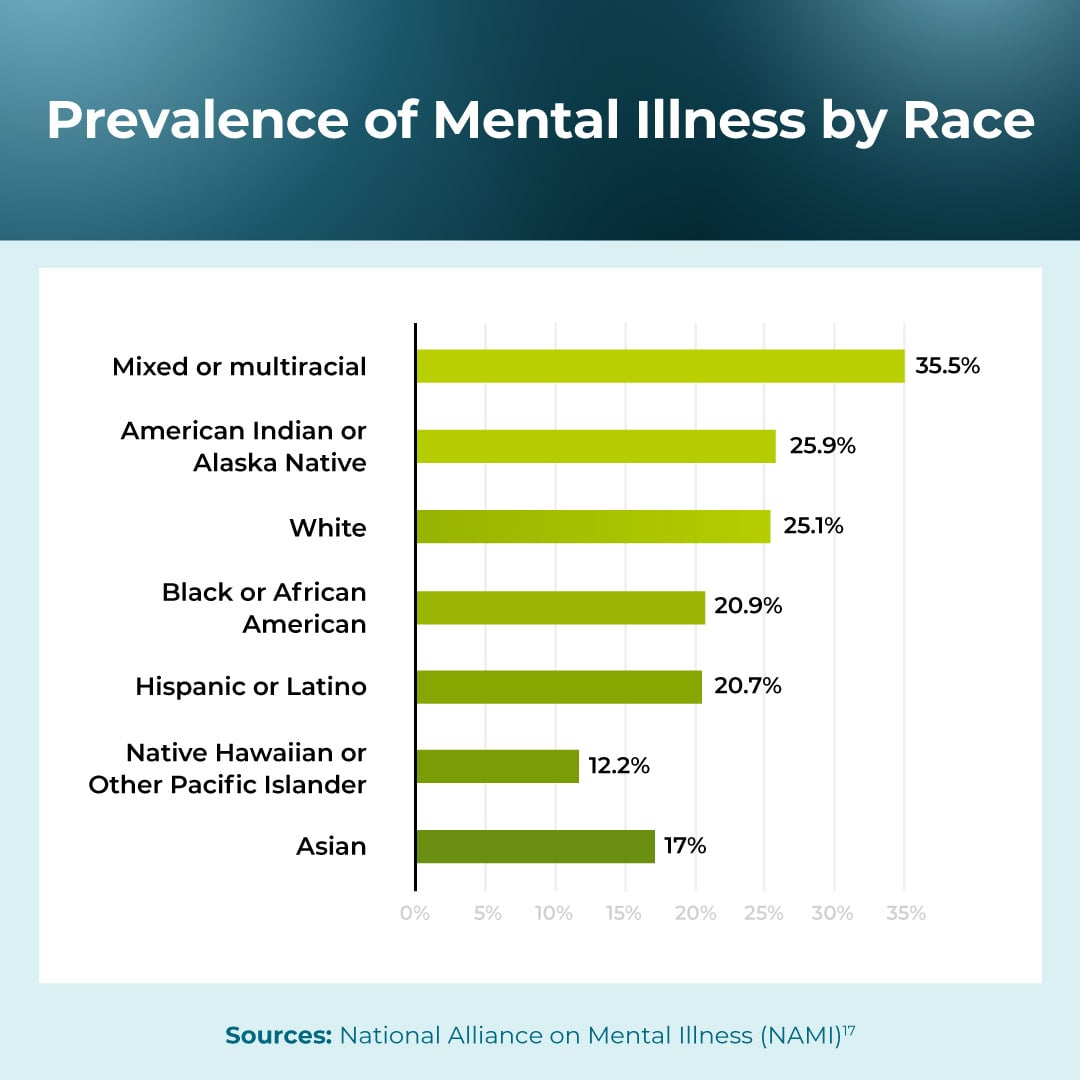
The Substance Abuse and Mental Health Services Administration (SAMHSA) is a government organization that collects data on substance use and mental health, including information for different racial groups. They found that the highest reported instances of mental illness in a given year within one race are within the American Indian or Alaska Native group at 25.9 percent.17 For those who identify as mixed race or multiracial, approximately 35.5 percent have a mental illness.17
- Mixed or multiracial: 35.5%17
- American Indian or Alaska Native: 25.9%17
- White: 25.1%17
- Black or African American: 20.9%17
- Hispanic or Latino: 20.7%17
- Native Hawaiian or Other Pacific Islander: 12.2%17
- Asian: 17%17

How Mental Illness Affects Individuals
Living with a mental illness can affect people in different ways. Much like the biopsychosocial model, the reported information shows how mental illness can take a toll on a person’s biology, social life and psychology. For example, the data below shows how a person’s mental illness can affect employment, which can lead to situational depression.6
- Children ages 6-17 are about three times more likely to repeat a grade if they have mental, emotional, developmental or behavioral problems.18
- 9% of U.S. adults with mental illness are unemployed compared to 4.3% of U.S. adults without mental illness.17
- 5% of adults with a mental illness also reported a substance use disorder.17
- Those with a severe mental illness have a life span 10 to 25 years shorter than the general population.19
How Mental Illness Affects Communities
Communities are also affected by mental illness. Mental health issues can lead to increased hospitalizations and economic challenges. Many unhoused people in communities around the country also struggle with mental illness.
- There are over 771,480 unhoused people in the United States,20 and 67% are reported to have a mental illness.21
- In 2024, over 8.38 million hospital emergency department visits in the U.S. were from substance use, highlighting how widespread these issues are.22
- Mental health issues result in $282 billion in costs each year.23
The Impact of COVID-19 on Mental Health
At the start of 2020, the world faced many challenges due to the COVID-19 pandemic. To help stop the spread of the virus, many people practiced social distancing, socialized less and started working from home. During this time, many people struggled with mental health and substance use issues. In 2020:
- 12% of adolescents and 4.9% of adults had serious thoughts of suicide.24
- 17% of adolescents aged 12 to 17 said they experienced a major depressive episode during the first year of the pandemic, compared to 8.4% of adults.24
- 3% of adults with a mental illness perceived the pandemic harmed their mental health.24
- 7% of adults say they weren’t able to get the mental health services they needed, which had a moderate to severe impact on their health.24


Mental Illness and Criminal Justice System Statistics
The reality is that many people in jails and prisons have mental illnesses. Aspects of having a mental illness include changes in emotion, thinking or behavior.3 Understanding this may shed light on new perspectives of incarcerated individuals.
- An estimated 44% of those in jail and 37% of those in prison have a mental illness.25
- Individuals with an untreated mental illness are 16 times more likely to be killed by the police.26
- Suicide is the leading cause of death in jails.27


Mental Illness in Rural Communities
It’s important to discuss mental illness in more rural areas because these communities have additional challenges. An estimated 60% of rural Americans live in areas with a shortage of mental health professionals.28 In 2021:
- 21% of adults in nonmetropolitan areas experienced symptoms of mental illness.17
- 6% of adults in nonmetropolitan areas have a serious mental illness.17
- 5% of people in nonmetropolitan areas had serious thoughts of suicide.17
Suicide Statistics
Suicide is often a tragic result of mental health problems. Sometimes, suicide happens after years of struggling with a mental illness like depression. Still, it can also be attributed to situational issues that pass, like the end of a relationship or money problems.29 Understanding suicide statistics may help communities be more aware of the challenge and provide support for those in need.
- Nearly 13 million adults had serious thoughts about suicide in 2022.30
- 49,316 people died by suicide in 2023.30
- Suicide rates increased by approximately 36% between 2000 and 2022.30
- 5 million adults made a suicide attempt in 2022.30


The United States Needs More Mental Health Workers
With millions of people experiencing mental illness in the United States, there’s a need for more mental health workers. Additionally, social workers, psychologists and healthcare workers often interact with those who have a mental illness.
Pursuing a Master of Science in Nursing (MSN) allows you to launch a career that supports national mental health. Earning an MSN with a role specialty in Psychiatric Mental Health Nurse Practitioner (PMHNP) at the University of St. Augustine for Health Sciences (USAHS) is a great path to become a Psychiatric Mental Health Nurse Practitioner, a trained mental health practitioner.
Request information about how a graduate degree in the health sciences can offer a rewarding career in mental healthcare.
Sources:
- “Mental Illness,” National Institute of Mental Health (NIMH), updated September 2024, https://www.nimh.nih.gov/health/statistics/mental-illness.
- “How Someone With A Mental Health Condition Can Qualify For Social Security Disability Benefits,” National Alliance on Mental Illness (NAMI) Iowa, 2026, https://namiiowa.org/how-someone-with-a-mental-health-condition-can-qualify-for-social-security-disability-benefits/.
- “What is Mental Illness?” American Psychiatric Association (APA), last reviewed July 2025, https://www.psychiatry.org/patients-families/what-is-mental-illness.
- “Biopsychosocial Model and Case Formulation,” PsychDB, , last edited January 27, 2024, https://www.psychdb.com/teaching/biopsychosocial-case-formulation.
- “Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR),” American Psychiatric Association (APA), 2026, https://www.psychiatry.org/psychiatrists/practice/dsm.
- “Situational depression or clinical depression,” Medical News Today, last medically reviewed July 28, 2022, https://www.medicalnewstoday.com/articles/314698.
- “Any Anxiety Disorder,” National Institute of Mental Health (NIMH), https://www.nimh.nih.gov/health/statistics/any-anxiety-disorder.
- “The State of Mental Health in America” Mental Health America (MHA), 2025, https://mhanational.org/wp-content/uploads/2025/09/State-of-Mental-Health-2025.pdf.
- “Major Depression,” National Institute of Mental Health (NIMH), last modified July 2023, https://www.nimh.nih.gov/health/statistics/major-depression.
- “How Common Is PTSD in Adults?,” PTSD: National Center for PTSD, U.S. Department of Veterans Affairs (VA), March 26, 2025, https://www.ptsd.va.gov/understand/common/common_adults.asp.
- “Bipolar Disorder,” National Institute of Mental Health (NIMH), https://www.nimh.nih.gov/health/statistics/bipolar-disorder.
- “Personality Disorders,” National Institute of Mental Health (NIMH), https://www.nimh.nih.gov/health/statistics/personality-disorders.
- “Eating Disorders,” National Institute of Mental Health (NIMH), https://www.nimh.nih.gov/health/statistics/eating-disorders.
- “Obsessive-Compulsive Disorder (OCD),” National Institute of Mental Health (NIMH), https://www.nimh.nih.gov/health/statistics/obsessive-compulsive-disorder-ocd.
- “Advancements in the Management of Schizophrenia,” PowerPak, May 1, 2024, https://journalce.powerpak.com/ce/advancements-in-the-management-of-schizophrenia.
- “Warning Signs of Mental Illness,” American Psychiatric Association (APA), last reviewed July 2025, https://www.psychiatry.org/patients-families/warning-signs-of-mental-illness.
- “Mental Health By the Numbers,” National Alliance on Mental Illness (NAMI), 2025, https://www.nami.org/mental-health-by-the-numbers/.
- “National Survey of Children’s Health,” Data Resource Center for Child & Adolescent Health, https://www.childhealthdata.org/browse/survey/results?q=9463&r=1&g=1023.
- Andrea Fiorillo, et al., “The Relationship between physical and mental health: an update from the WPA Working Group on Managing Comorbidity of Mental and Physical Health,” World Psychiatry, January 14, 2023, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9840511/.
- Soucy, Daniel, et al., “State of Homelessness: 2025 Edition,” National Alliance to End Homelessness, September 4, 2025, https://endhomelessness.org/state-of-homelessness/.
- Harris, E., “Two-Thirds of Unhoused People Have Mental Health Disorders,” Journal of the American Medical Association, May 10, 2024, https://jamanetwork.com/journals/jama/article-abstract/2818774.
- “National Estimates From Drug-Related Emergency Department Visits, 2024,” Drug Abuse Warning Network (DAWN), 2024, https://www.samhsa.gov/data/sites/default/files/reports/rpt56252/dawn-national-estimates-2024.pdf.
- Sperling, J. “Mental Health and the Economy — It’s Costing Us Billions,” Columbia Business School, May 28, 2024, https://business.columbia.edu/insights/business-society/mental-health-and-economy-its-costing-us-billions.
- “Key Substance Use and Mental Health Indicators in the United States: Results from the 2020 National Survey on Drug Use and Health,” The Substance Abuse and Mental Health Services Administration (SAMHSA), October 2021, https://www.samhsa.gov/data/sites/default/files/reports/rpt35325/NSDUHFFRPDFWHTMLFiles2020/2020NSDUHFFR1PDFW102121.pdf.
- “About Criminal and Juvenile Justice,” The Substance Abuse and Mental Health Services Administration (SAMHSA), May 24, 2024, https://www.samhsa.gov/communities/criminal-juvenile-justice/about.
- “Overlooked in the Undercounted: The Role of Mental Illness in Fatal Law Enforcement Encounters,” Treatment Advocacy Center (TAC), https://www.treatmentadvocacycenter.org/reports_publications/overlooked-in-the-undercounted-the-role-of-mental-illness-in-fatal-law-enforcement-encounters/.
- Wang, L., “Rise in Jail Deaths Is Especially Troubling as Jail Populations Become More Rural and More Female,” Prison Policy Initiative, June 23, 2021, https://www.prisonpolicy.org/blog/2021/06/23/jail_mortality/.
- “Rural mental health resource center,” Mental Health America (MHA), 2026, https://mhanational.org/rural/.
- “Suicidal thoughts and suicide prevention,” Mind, July 2025, https://www.mind.org.uk/information-support/types-of-mental-health-problems/suicidal-feelings/causes-of-suicidal-feelings/.
- “Facts About Suicide,” Centers for Disease Control and Prevention (CDC), last modified March 26, 2025, https://www.cdc.gov/suicide/facts/index.html.