Collaboration is the hallmark of creative problem-solving, shared expertise and deeper understanding. In healthcare, interprofessional teams can improve patient outcomes and enhance patient care.
According to the World Health Organization (WHO), interprofessional education (IPE) is an experience that “occurs when students from two or more professions learn about, from, and with each other.”
Norman Belleza, PT, DPT, PhD, Assistant Professor, PT Programs at The University of St. Augustine for Health Sciences (USAHS), authored an article for Inside Higher Ed, highlighting the impact of interprofessional education on the future of healthcare.
“When health-care education programs train students to be good collaborators, the entire health-care system improves—and can be greater than the sum of its parts,” writes Dr. Belleza.
In healthcare, the effort to achieve patient well-being and “everyday miracles” is often collaborative, Dr. Belleza explains. He sees this process as beneficial due to individual providers’ ability to pool their specialized knowledge and ultimately improve lives.
Alternatively, in postsecondary education, programs often operate in silos. “Different health-care specialties—such as speech-language pathology, physical therapy, occupational therapy and nursing—are taught as though they each function independently,” Dr. Belleza writes.
He sees this compartmentalization in a complex field as an obstacle to the full potential of holistic patient care. “The result? Too many missed opportunities to harness the full healing power of interprofessional collaboration—an oversight that directly impacts patient outcomes.”
Dr. Belleza attests that there’s a better way. He advocates that to nurture the synergy of diverse healthcare disciplines, we should integrate interprofessional education (IPE) into the curriculum from the beginning. A patient’s needs extend beyond one discipline. This process allows healthcare practitioners to recognize their strengths and limitations and partner to provide patient-centered care.
“By empowering health care professionals who can seamlessly collaborate across disciplines, IPE can ultimately enhance patient outcomes and reshape the health-care landscape,” says Dr. Belleza.
IPE has the potential to make patient care more culturally competent and accessible. Dr. Belleza claims that a well-coordinated, cross-disciplinary education can prepare healthcare practitioners to alleviate health disparities in underserved communities, eliminate gaps and redundancies in care, prevent diagnostic errors and reduce overbilling.
“Training under an IPE model can replicate the experience of working in multidisciplinary practices such as at free clinics, where such communities tend to receive services,” says Dr. Belleza.

So, how do we implement IPE?
Dr. Belleza envisions three cornerstones of success: creativity, intention and commitment.
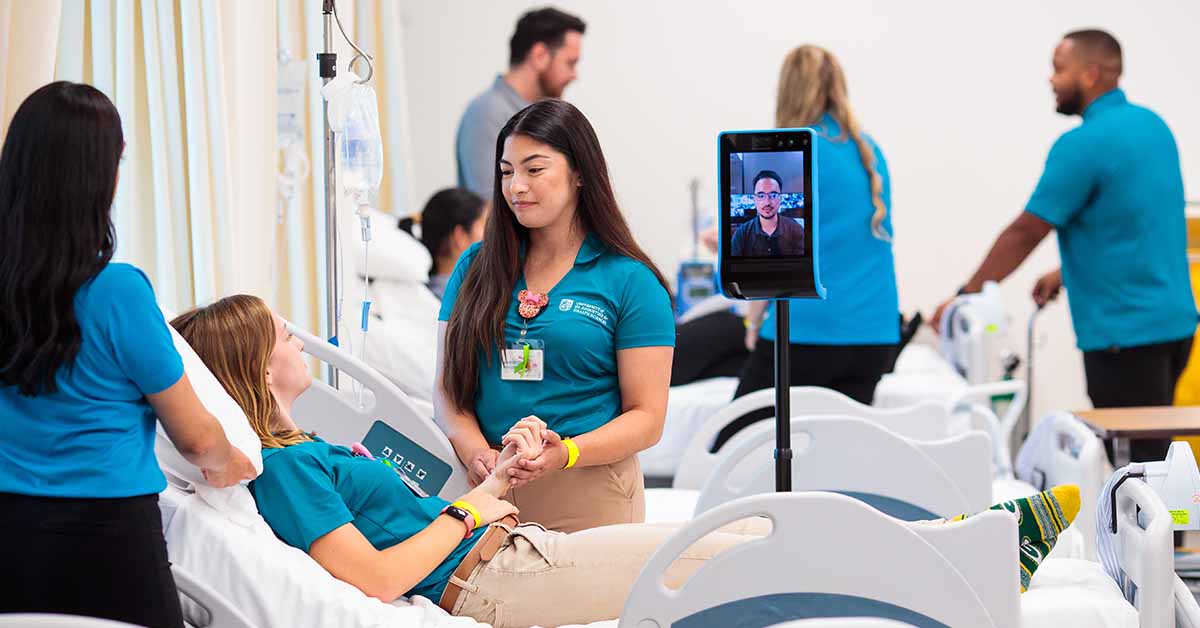
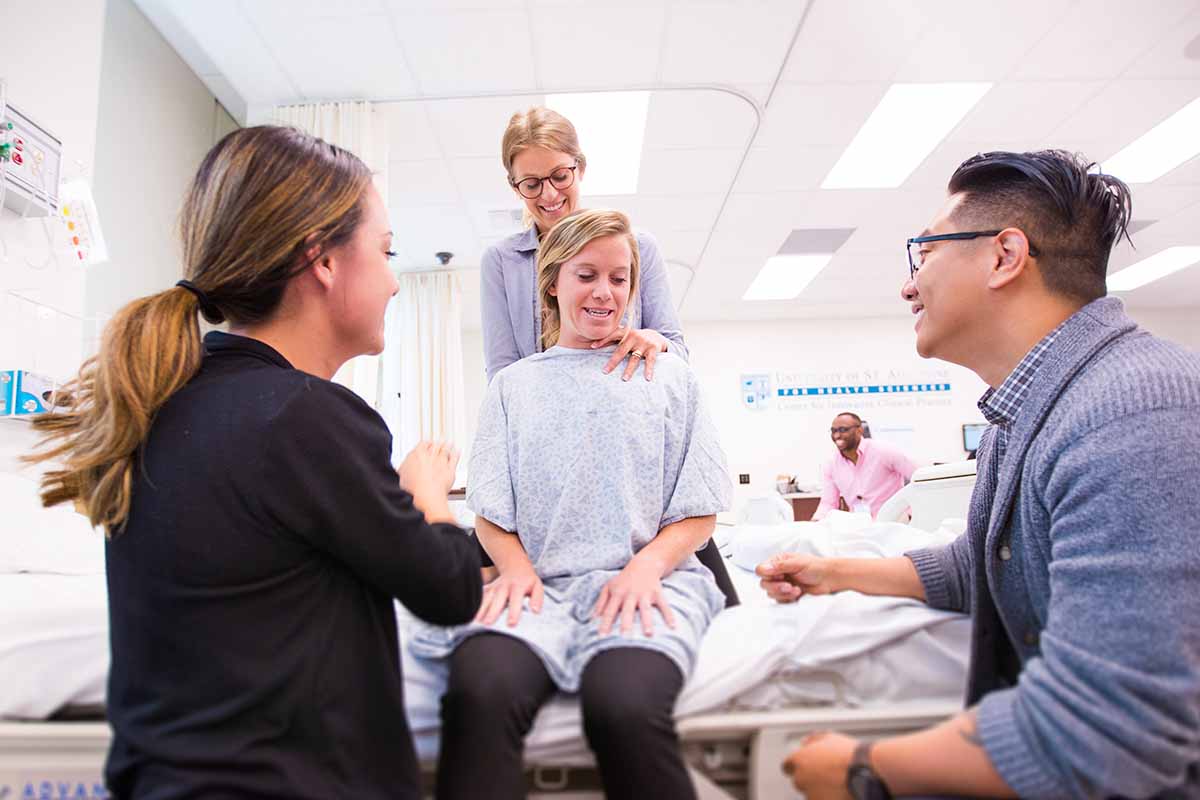
He calls for simulation labs such as USAHS’ Center for Innovative Clinical Practice (CICP), faculty collaboration, community health fairs and clinical rotations.
According to Dr. Belleza, scaling IPE is an effort facilitated by cohorts, repetition and team building.
Are we ready to reimagine how we educate the next generation of healthcare leaders?
The time is now, and IPE is critical to the evolution of healthcare, according to Dr. Belleza.
“Making IPE a priority today in health-care education can help create a pipeline of skilled, adaptable practitioners far into the future, practitioners who can find the right solution for a given patient not just within the arsenal their discipline maintains, but within any arsenal, from any discipline,” he says.
Read Dr. Belleza’s article for Inside Higher Ed.
Are you ready to pursue an interprofessional education through USAHS’ immersive, collaborative graduate health sciences programs? Request more information or apply today.