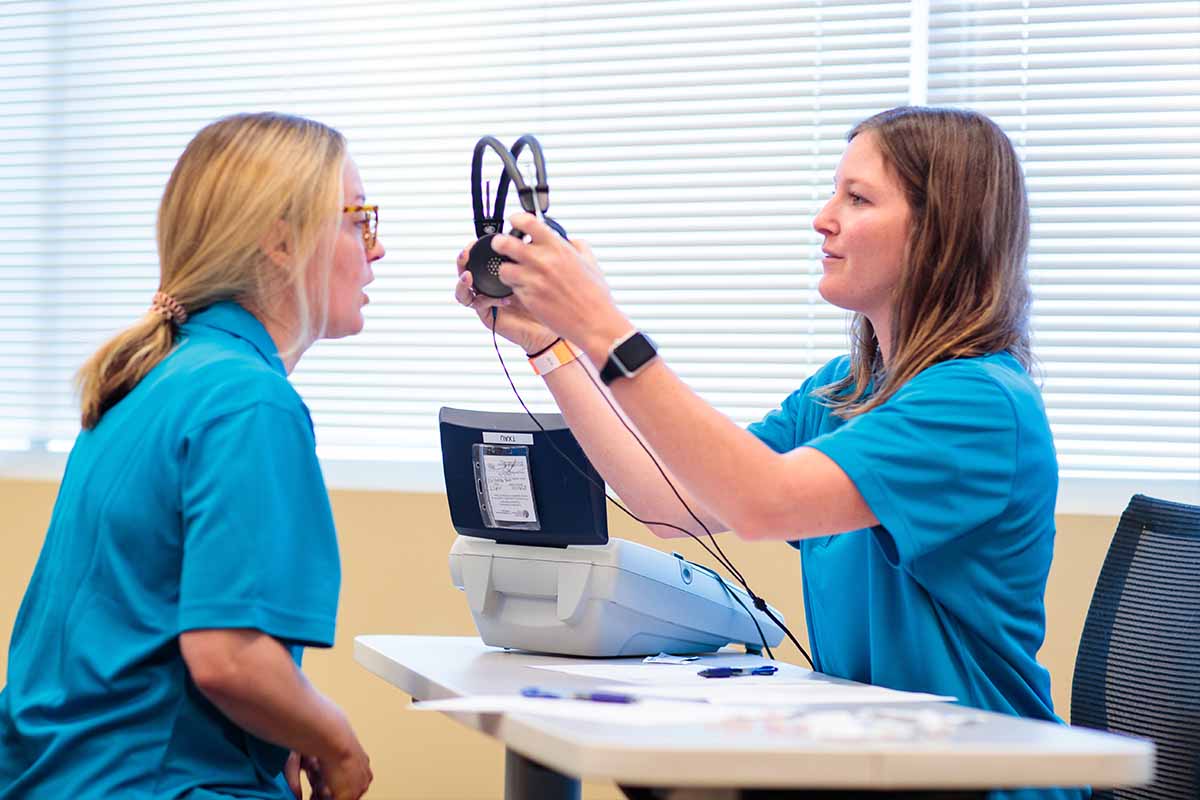
USAHS now has a Double 3 telepresence robot from Double Robotics on each of our five campuses. Faculty across programs can begin using this cutting-edge technology in their simulation classes in our Centers for Innovative Clinical Learning (CICPs), as well as other learning contexts.
The Double 3 telepresence robot is a recent advancement in telehealth that enables a remote healthcare provider to communicate with a patient or other member of the care team through a movable robot that provides a human-like virtual presence through a screen. Remote providers can use the robot to collaborate with an interdisciplinary team via case conference. An occupational therapist (OT), student, or other healthcare professional located anywhere in the world can consult with a patient by remoting into the robot. They can maneuver the robot around the patient and can ask the patient to move, so they can assess movement and mobility.
For the practitioner, the robot offers better engagement opportunities than other telepresence options, as well as the chance to feel more present in that interaction. For the patient, it offers a more seamless experience of a human presence than does a static screen. Check out this video to see the Double 3 in action.
How We Use the Robots
“We wanted to have a telepresence within our simulations: the chance to bring in a remote healthcare practitioner,” says Dr. Elisabeth McGee, DPT, MOT, manager of the University’s CICPs. Telehealth, including teleOT and telePT, is an emerging healthcare approach that is growing in importance. “We want our students to be prepared, to be on that cutting edge of technology where they’re comfortable interacting with someone who is remoting in.”
The robot enables intraprofessional collaboration between students and mentors in the same field, as well as interprofessional collaboration across disciplines. It also allows distance students and practitioners to engage in simulations with in-person students. “We’re bridging the gap between education and practice,” says Dr. McGee.
From Pilot to Permanent
Faculty saw the Double robot demoed at the International Meeting on Simulation in Healthcare (IMSH) and wrote a funding proposal through the University’s Innovation Steering Committee. They launched the Double robot as a pilot in Summer 2019 in the MOT/OTD Clinical Applications in Geriatrics course. The pilot has run for three consecutive trimesters.
On our St. Augustine, Florida, campus, this course is taught by assistant professor Kelly Layne, OTD, MOT. Students participate in a simulation scenario in which an OT student has the opportunity to consult with an ALS expert about the treatment of a mock client who has ALS.
Dr. Layne has been collaborating since 2017 with that expert, Dr. Helen Carey, PhD, MScOT, a guest faculty member from Glyndwr University in Wales. The two professors have been running synchronized case study sessions that help both groups of students gain insight into the occupational therapy context of their respective countries. They had been videoconferencing using What’s App and Facebook Live, but between technical difficulties with those services and the promise of the expanded capabilities of the Double robot, they were excited for the chance to pilot the robot.
Dr. Carey remoted in with the robot and examined the simulated patient, who was resistant to following directions, so Dr. Carey modeled a skillful response. After the immersive simulation, Dr. Carey offered feedback to the student and patient. Dr. Layne says, “Students felt like they had met her, like it was the same as her being here.” The pilot was successful, garnering positive feedback from students and faculty.
The Double Robot UX
To remote in, the user experience (UX) is easy; you come into the Double 3 app through a link. You use arrows on your computer keyboard and sliders on the screen to move forward and back; turn corners; and raise, lower, and tilt the robot. Dr. Carey says it takes a little practice to get the moves right. “I’ve gotten better at seeming more human, less rigid,” she says. “But I also have to move in an understated way to be less distracting to students.”
She continues, “You do have the eye contact and can ask questions directly of the patient. But personal space can be challenging to gauge. You don’t have that feedback.” To mitigate that issue, she tells the patient, “Let me know when I’ve gotten close enough.”
Advantages over Other Communication Methods
Faculty say that the Double robot is better than consulting with a professional via email because you can see the patient, and communication is synchronous. It’s better than phone because you can see the patient. It’s better than videoconferencing because the consultant is in control of the technology. The consultant can more easily develop rapport with the patient, get a better sense of their actual presence. They don’t have to ask the patient or the local practitioner to “move the camera” all the time.
The robot is ideal for use with small groups and when the consultant should control the camera. However, videoconferencing is preferred for teaching a larger class and when you need a wider view of the remote practitioner beyond a headshot. Both, of course, save travel expenses compared to in-person consultation.
Other Uses of the Robot
In a subsequent session, Dr. Layne conducted an interprofessional simulation with the class: A physician “running late” remoted in with the robot and participated in a case conference simulation, together with students from other programs. And at the end of the term, Dr. Carey used the robot to remotely read and grade poster presentations of students on the St. Augustine campus.
Although the robot was piloted in an OT course, one robot per campus is now available for faculty to use across departments. At the Family Nurse Practitioner clinical intensive on the St. Augustine campus, a faculty member from another campus remoted in with the robot and consulted with students on wound debridement, assessing, and treating.
As Dr. Layne says, “What you can do with this robot is limited only to your imagination.”