
At a time when so many aspects of education are compelled to go online, USAHS faculty are not only adapting—we’re taking virtual learning to the next level. During Fall 2020, faculty members across departments collaborated to create clinical simulation sessions that were delivered in a live, interactive virtual mode. Filmed with live actors in the Center for Innovative Clinical Practice (CICP) on the San Marcos campus, the simulations leveraged gaming technology, virtual escape rooms, and 360-degree virtual clinical environments. They brought students from across programs and campuses together to solve patient problems in interprofessional teams.


One virtual simulation (VSim) was particularly timely: The case study of a fictional patient, Andrew Carino, who is in the ICU with COVID-19. Andrew comes in with dangerously low oxygen saturation levels and a history of underlying conditions. He is sedated and placed on a ventilator, as well as a chest tube and a feeding tube. He is also on oxygen and has two IV lines.
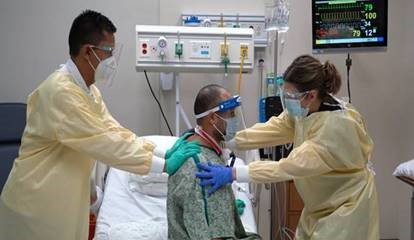
This simulation centered the roles of an occupational therapist and physical therapist, played by faculty members. Their treatment goals are to help Andrew sit at the bedside, get dressed while seated, and stand up with an Eva walker. While doing so, they must properly manage all his lines and leads. Andrew can’t speak because of the intubation, so he uses a communication board, bringing in the role of speech-language pathology. Multiple machines are beeping, building the stress level. When Andrew’s oxygen level drops, the OT and PT need to call in a nurse.
Faculty as Movie Directors
“Students love it,” says Maureen Johnson, PhD, MS, OTR/L, an assistant professor in the occupational therapy programs on the USAHS San Marcos campus. “People think of online learning as just watching a PowerPoint. But this is cutting-edge technology. It’s fun, funny, and cool. And having a COVID-19 patient is so true to life.”
Norman Belleza, PT, DPT, an assistant professor of physical therapy on the San Marcos campus, wrote the script for the COVID-19 simulation. Dr. Johnson (who is affectionately known as “Dr. Mo”) helped to fine-tune it. “Mo and I had so much fun doing this,” Dr. Belleza says. “It was just tremendously fun.”
Elizabeth Horsely, RN, MSMS, provided input on the medical details of COVID-19 and the nursing aspect of the simulation. Nickole Hines-Staples, MA, CCC-SLP, offered feedback from the speech-language pathology side. Clinical simulations specialist Mechelle Roy helped create the simulated ventilator and prepare the CICP for filming. The team worked fast to create the VSim within just two weeks.
“It’s almost like creating a movie script,” Dr. Belleza says. “We’re thinking about where to put the camera, which devices to use, and how to scaffold the activities so they build logically on each other. It is a lot to handle, though, being a writer, director, and actor.”

Spearheaded by Elisabeth McGee, DPT, MOT, PT, OTR/L, manager of the Centers for Innovative Clinical Practice, USAHS hosted five multi-campus VSims during the Fall term. Along with interprofessional education, the scenarios emphasized patient safety and culturally responsive therapeutic approaches. In one scenario, a patient in a same-sex marriage undergoes gender reassignment/confirmation surgery. In another simulation, students work as an interprofessional team to deliver safe, evidence-based patient care in a cardiopulmonary trauma setting. Students interact with 360-degree and gaming technology as they make decisions about patient care.
How Students Participated


In the COVID-19 simulation, students watched a video laying out the scenario, then joined breakout groups with other students from our OT, PT, SLP, and nursing programs to work on activities together. First was a virtual escape room: In a 360° treatment room environment, students had to identify pieces of equipment and write out their names in hangman-style puzzles. Uncovering hidden letters gave the escape code.
Next, students participated in a branching scenario with multiple-choice questions animated by speaking avatars of Drs. Belleza and Mo, created using gaming technology. Dr. Belleza describes these questions as “stop-points for you to decide the best choice of intervention based on events unfolding within the simulation.”
Student feedback has been overwhelmingly positive. “Thank you so much for this great interactive experience,” one student wrote. “I enjoyed observing as well as being involved with my team.”
A DPT student commented, “One of the big reasons I chose USAHS was for the interdisciplinary aspect. I am super passionate about seeing these sims and the collaboration grow.”
Drs. Belleza and Mo also worked together to create in-person interprofessional simulations as part of Patient/Client Care Management 1, a first-trimester core course for the DPT, MOT, and OTD programs on all campuses. In response to the pandemic, they designed virtual versions of those simulations, which they will present at the World Physiotherapy Congress 2021. As thought leaders in the field of healthcare simulation, they will give a similar presentation at this year’s International Meeting on Simulation in Healthcare (IMSH).
“We’re taking virtual learning to the next level,” Dr. Belleza says. “It’s great. And it requires a lot of effort and time.”








