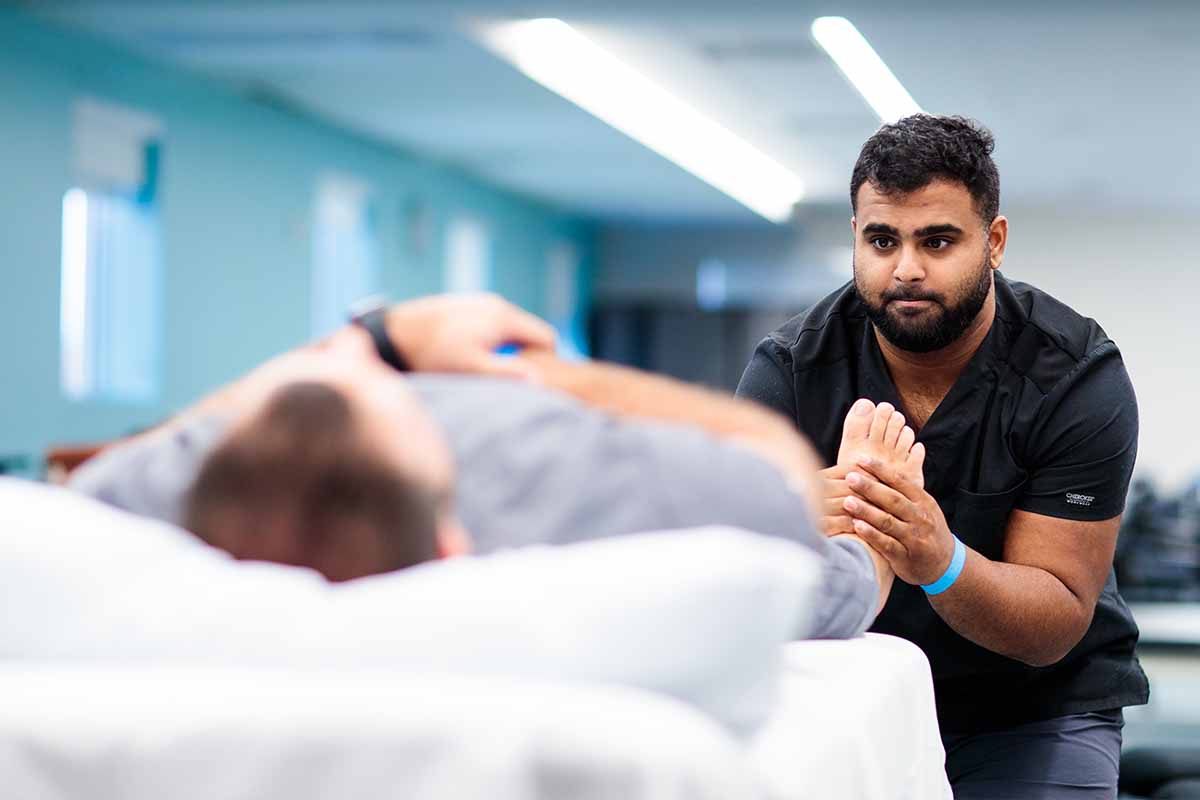
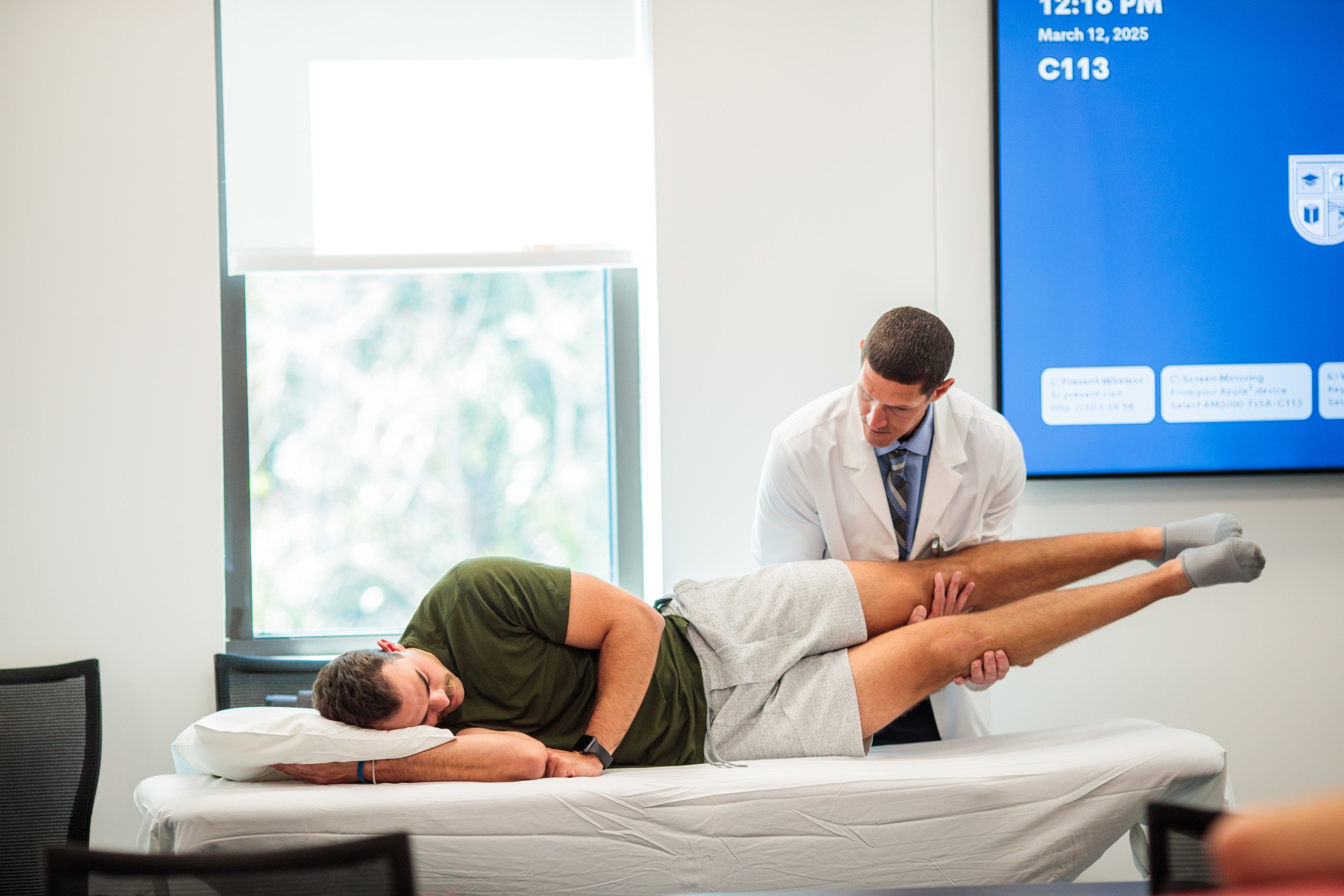
Pictured: Students help practice balance with this patient who recently had a fall.
On her first day as a student in the pro bono clinic on USAHS’ St. Augustine campus, Allison Esposito was assigned to work with a patient who had a transfemoral amputation and a prosthetic leg. “I was kind of terrified at first,” she says. As a sixth-trimester student in the Doctor of Physical Therapy program, she had completed one clinical rotation but had not yet worked with a patient who had a prosthesis.
St. Augustine’s pro bono clinic is interprofessional, meaning that students from our occupational therapy and physical therapy programs work together. Dr. Esposito (who is now a licensed physical therapist, having graduated Dec. 2020) worked with an OT student to assess the patient, then design and implement a treatment plan.
“He had a fear of descending the stairs,” Dr. Esposito says. “He had to coordinate his prosthesis with that task, slamming the heel back to lock it out at the knee so it wouldn’t buckle. He also would lose endurance going up the stairs. We wanted to help him get his confidence back up.” Dr. Esposito worked with the patient to strategize about the best biomechanics for ascending and descending the stairs. “He was open and willing to show me movements that work best for him,” she says. In turn, the OT student helped the patient find household objects that he could use to help him grip railings at home and out in public.
“The experience was amazing,” Dr. Esposito says. “To see what the OT had to offer in terms of adaptive equipment. PT might tend to order braces—but this patient didn’t have money. OTs get a little more creative. You don’t realize how much the two fields are related. They play off each other.”
She says that working with this patient taught her a lot. “Now I’m more comfortable and confident working with people with prostheses.”
Working Side by Side

Pictured: Students are creating an orthotic device for this patient who is a guitarist.
The seeds for the St. Augustine pro bono clinic were planted about 15 years ago, when students began treating patients within an elective DPT course. In 2017, it became a true pro bono clinic, bringing real patients referred by the neighboring Flagler Hospital and other healthcare organizations into a double-sized classroom on campus. DPT students in the sixth-trimester course Musculoskeletal IV: Clinical Reasoning began working in the clinic, and soon thereafter, OT students from the fourth-trimester course Clinical Applications in Adulthood joined. Currently, rotating through the pro bono clinic is part of the required curriculum for all DPT and OT students.
Kaitlyn Cremer, OTD, MOT, OTR/L, describes the clinic as “two very different programs coming together in a unique learning experience that serves the community.” Dr. Cremer is one of five faculty members who lead the clinic, along with her sister Lydia Cremer Kite, MOT, OTR/L; Todd Bourgeois, PT, DPT, PhD; Garrett Mandel; PT, DPT; and Lindsay Perry, PT, DPT.
“PT and OT students work side by side like in a real clinic,” Kite explains. “There’s a waitlist for these classes every semester. It’s great to see.”
Faculty recruit patients, most of whom lack health insurance and are underserved by the system. Kite and Dr. Bourgeois triage the patients to determine whether they need PT, OT, or both. For those who need both, students are paired up to assess the patient together and come up with a joint treatment plan, learning each other’s roles in the process. “We want students to talk to each other and figure out how to work interprofessionally on their own,” Dr. Cremer says. “But these conversations are usually facilitated by faculty. Students are also learning their own profession at the same time.”
Alumnus Lee Richards, DPT, was a student in the pro bono clinic. “It was essentially one-on-one mentoring with real patients,” he says. “The faculty took a hands-off approach as instructors unless you needed guidance. Then they would get you to think about things in different ways.” Students also get practice working with an electronic medical record system: scheduling patients, documenting their plan of care, and discharging them. “Faculty gave us really good critiques on our notes,” Dr. Richards says.
Challenges and Rewards
According to Kite, the clinic’s faculty members meet weekly to discuss specific cases, especially complicated ones. “We’ve become a family who constantly work together,” she says.
“Stuck together, in my opinion!” Dr. Cremer laughs.
Dr. Bourgeois says that managing the clinic is time-consuming, and faculty have had to handle regulatory, administrative, and other logistical issues. “There were barriers all over the place and we just kept jumping them,” he says, a fitting metaphor given that Dr. Bourgeois is a three-time national qualifying champion on the show American Ninja Warrior.
Running the clinic is also rewarding, Dr. Cremer says. “We’re not just academics—we’re practicing clinicians. We want to help people and teach our students how to help people. My two loves come together in this clinic.”
“It’s good for students to see us treating patients,” she continues. “It makes the profession come to life for them. It improves their appreciation of us. And we can see the students’ passions, see their confidence grow.”


Pictured: Student helps patient with functional reaching and posture training.
Adapting for the Pandemic
Dr. Mandel says that after COVID-19 restrictions began in March 2020, the clinic had to go virtual. It is currently functioning with PT students only. Whereas PT students already have completed one clinical rotation before they enter the clinic, the OT students do not yet have fieldwork experience—and they need more practice before treating people via telehealth. For OT, Kite and Dr. Cremer have trained scripted actors to participate in a scaffolded telehealth simulation experience with students; they plan to run these simulations until COVID restrictions lift.
This situation does have an upside. “Students are realizing how much they can do in the virtual environment,” Dr. Mandel says. “They go into a breakout room with the patient, and mentors bounce between rooms.” When the pro bono clinic opens to in-person treatment again, they plan to keep a telehealth component.
“It’s amazing to see the fire that gets lit under the students as they get out of the textbook and into real life,” Dr. Mandel says. “This is a chance to have conversations not about black and white, but about the gray areas. Being able to work hand-in-hand with other professionals allows you to learn and grow. You understand how you are operating as a cog in the wheel of healthcare.”
A Case Study Worthy of a Presentation
Before the pandemic, Doctor of Occupational Therapy (OTD) student Nicole McMahon worked with a PT student to help a patient who had both low vision and thoracic outlet syndrome (TOS). Hunching over to read had contributed to causing the TOS. The PT student gave the patient a home exercise packet, but he couldn’t read it because of the tiny handwriting; the PT student reprinted the instructions in a larger font and performed manual manipulation on the patient to relieve the TOS.
Dr. McMahon (who is now a licensed occupational therapist, having graduated Dec. 2020) helped the patient find better body mechanics for reading. She also helped him change his office setup, which helped with both the low vision and the TOS. The TOS was causing insomnia, so Dr. McMahon worked with him on positioning for comfort and sleep. She checked in with Dr. Cremer, a low vision expert, for recommendations about vision exercises.
“I think the professions need each other,” Dr. McMahon says. “Speech, too.”
Dr. Cremer reports that this patient was discharged pain-free and able to sleep. She wrote up the case study into a presentation for the Envision Conference, an interprofessional gathering of low vision rehabilitation professionals and researchers. She gave a similar presentation to the Pro Bono Network Conference.
Applying Learning in Their Careers


Pictured: Patient was working on her occupation which includes sewing.
“I’m so grateful for this experience—that I learned to think in an interprofessional way before my fieldwork,” Dr. Esposito says. “I know what an OT is looking for, so I know when it’s appropriate to refer patients to an OT for part or all of their treatment.” She has just started a job as a PT in an outpatient pediatrics clinic in Atlanta, Georgia. She says she would like to set up a pro bono clinic someday, if she has the means and opportunity to do it.
Dr. Richards is applying what he practiced in the pro bono clinic within his current role at STARS Rehab in St. Augustine. He learned to find the patient’s limitation, perform a treatment, then remeasure the limitation—all in the same session. “It opened my eyes to what’s possible in an appointment,” he says. “For example, Dr. Mandel helped me with a patient who had plantar fasciitis. We found limited dorsiflexion in her ankle joint, and we helped her increase her range of motion and get to less pain with motion in just one session. That gave the patient more buy-in, because she saw improvement in the moment instead of through doing exercises over weeks.”
When asked his impressions of the faculty, Dr. Richards says, “I couldn’t imagine going through this clinic with anyone else. The faculty are so approachable and knowledgeable. They challenge you, make you think, see you grow.”
USAHS’ Miami and Austin campuses also run clinics for local community members, and plans are in the works to establish more. Check out these posts: