Simulation-based learning places students in situations where they can put their classroom knowledge into practice. In healthcare, simulation training has been part of curricula since the 18th century; it has been continually evolving as technology advances.
This post explores the history of simulation in healthcare, highlights its advantages over other methods of learning, details the types of simulation environments, and shows how simulation-based learning benefits healthcare providers, students, and patients.
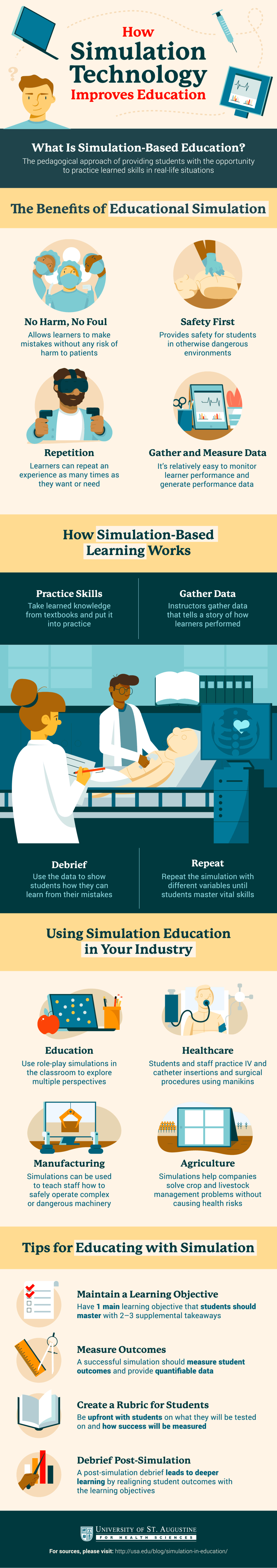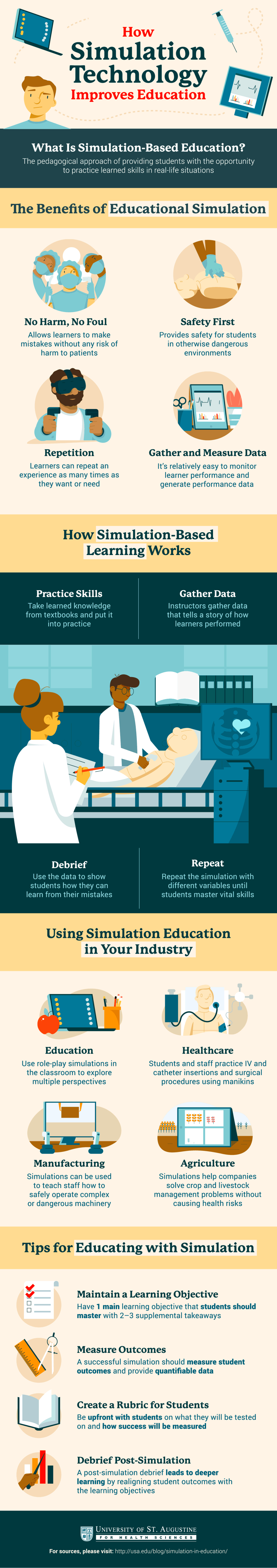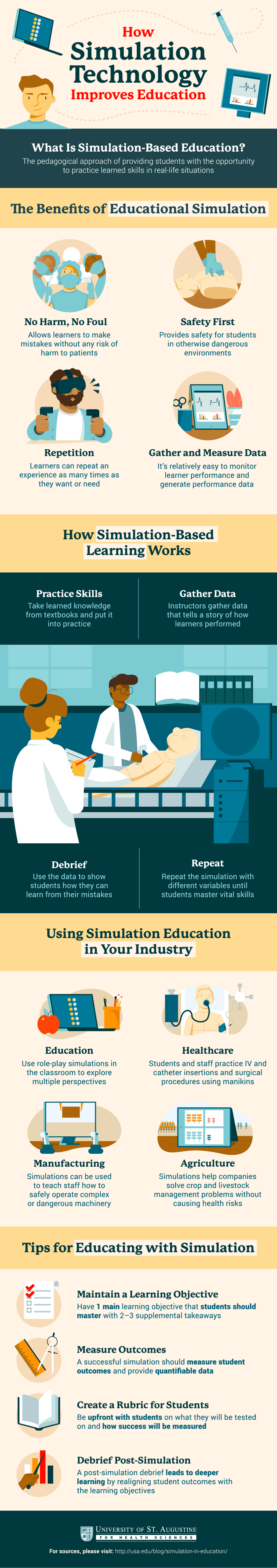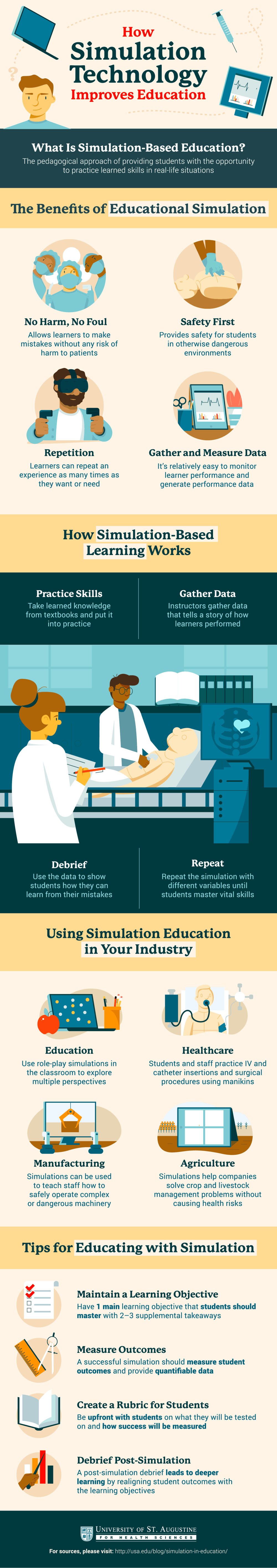
What is Simulation-Based Education?
Simulation-based education is the pedagogical approach of providing students with the opportunity to practice learned skills in real-life situations.
Source: BMC Medical Education 16, 152 (2016)
Educational simulation is a teaching method that tests participants’ knowledge and skill levels by placing them in scenarios where they must actively solve problems. The instructor defines the parameters to create a safe environment for hands-on learning experiences.
When participating in a scenario, students must quickly evaluate the situation, decide on the best course of action, and perform the correct procedural steps. Educators can then assess whether the students understand the material and are translating their learned knowledge into skills.
Simulation is useful not only for students—it can also be a way for patients to practice new skills while healthcare providers measure their progress.
History of Educational Simulation in Healthcare
The systematic use of simulation in healthcare education advanced in the 18th century in Europe. At that time, medical educators were improving the use of forceps in obstetrics. Obstetric simulators were created that could leak amniotic fluid and blood; midwives and obstetricians trained with these devices so they could better manage complications of childbirth and use forceps in optimal ways.
Simulation in medicine continued to advance during the 19th and 20th centuries. It was not until after the Industrial Revolution that technology developed to such a degree that simulation became a popular and standard feature of healthcare education. ((Harry Owen, “Early Use of Simulation in Medical Education,” Simulation in Healthcare: The Journal of the Society for Simulation in Healthcare, April 2012: https://journals.lww.com/simulationinhealthcare/Fulltext/2012/04000/Early_Use_of_Simulation_in_Medical_Education.4.aspx))
Advantages of Simulation-Based Learning
Turn Knowledge into Practice
Simulation-based learning allows students to apply abstract concepts to active hands-on practice. For instance, nursing students can read about how to perform a procedure, but hands-on practice will help them feel much more comfortable. Practicing with mock or real patients in a dedicated clinical environment such as a clinical skills lab helps students learn to make appropriate decisions at various points within the scenario, especially when patient complications occur.
For patients, simulation-based learning provides a way for them to practice daily tasks without putting themselves and others at risk. For example, someone learning to drive again after a serious injury can benefit greatly from driving in a simulator under the supervision of an occupational therapist before driving an actual vehicle. The simulator provides safety for the patient and others.
Gather Measurable Data on Students and Patients
Another benefit of simulation in healthcare education is the ability to gather measurable data on students and patients. In simulation-based learning, the instructor defines the parameters of the scenario, and based on these parameters, can gather data on the progress of students and patients.
The instructor can monitor how participants make decisions and how long specific actions take, thus gleaning information about which skills need further practice and how far participants are from mastering them. Having this information establishes a future safety net for those involved by not putting unprepared students and patients in risky situations outside of simulations.
Safety for Practitioners and Patients
Simulation learning allows students and patients to experience an analog of a real-life situation while keeping themselves and others safe. Students typically practice with a mock patient, such as a manikin or a scripted actor, so if they make mistakes in their treatment protocol, this won’t adversely affect a real person. And the instructor can step in if something goes awry.
For patients, simulations can help them build confidence in performing challenging movements before they need to do so independently in real life.
Examples of Simulation-Based Learning for Students
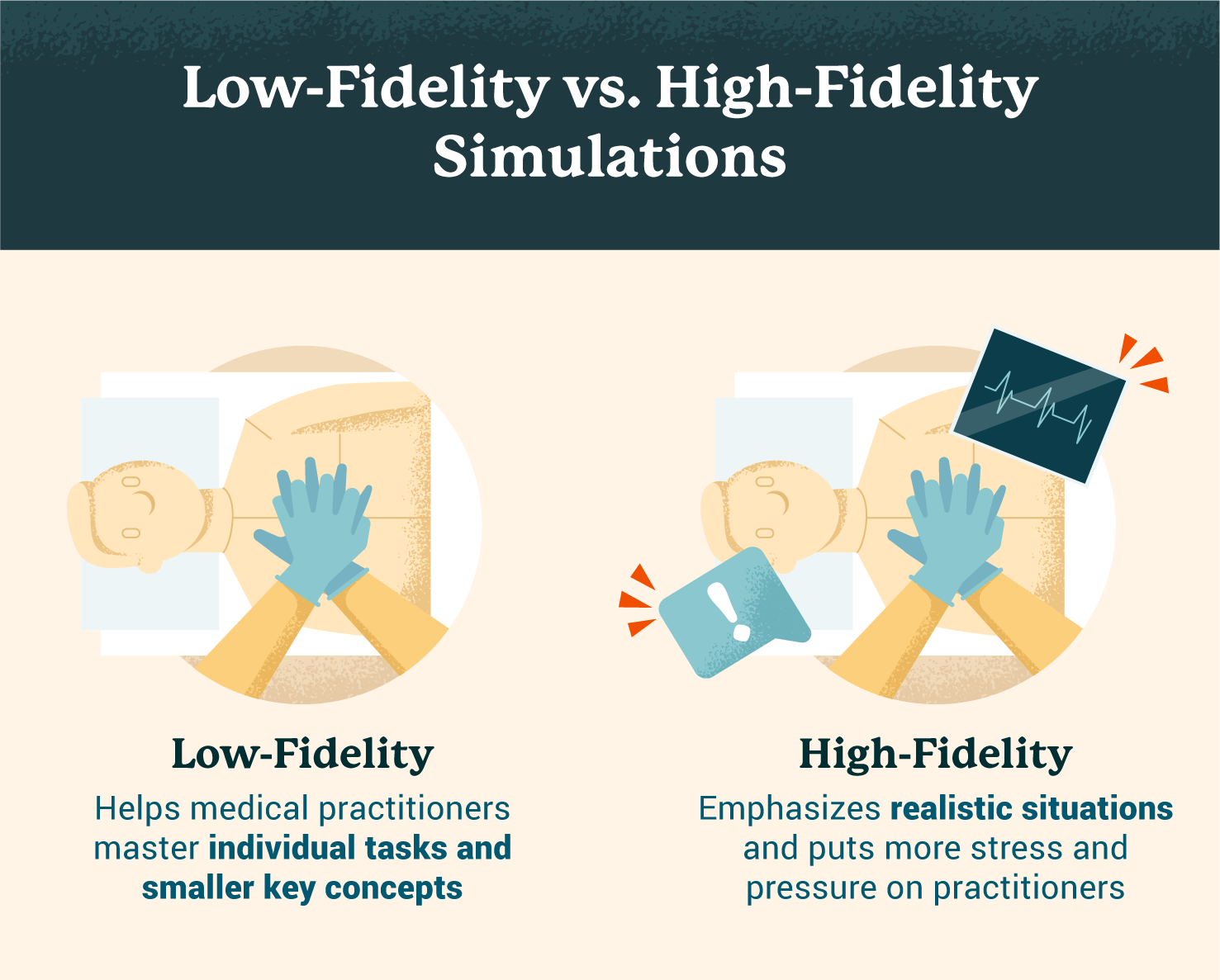

Low-Fidelity Simulations for Students
A low-fidelity simulation (LFS) imitates an actual situation but simplifies the variables. The purpose of an LFS is to turn learned knowledge into a technical skill. LFSs can be both hands on and computer or written-based scenarios. By removing some of the factors that can be present in a real-life situation, students in an LFS can better understand and practice more discrete concepts.
For instance, when a student learns how to perform cardiopulmonary resuscitation (CPR), the first step is understanding how many chest compressions versus breaths to administer over a certain period of time. The second step, and where you need a simulation manikin, is knowing where to perform the chest compressions and with how much pressure, depending on whether the patient is a baby, child, or adult. Using a CPR manikin aids students in learning the technical skill of chest compressions. A textbook can explain how to do chest compressions, but practice is essential. Again, LFSs do not overwhelm the student with other real-life factors.
Other examples of LFS include:
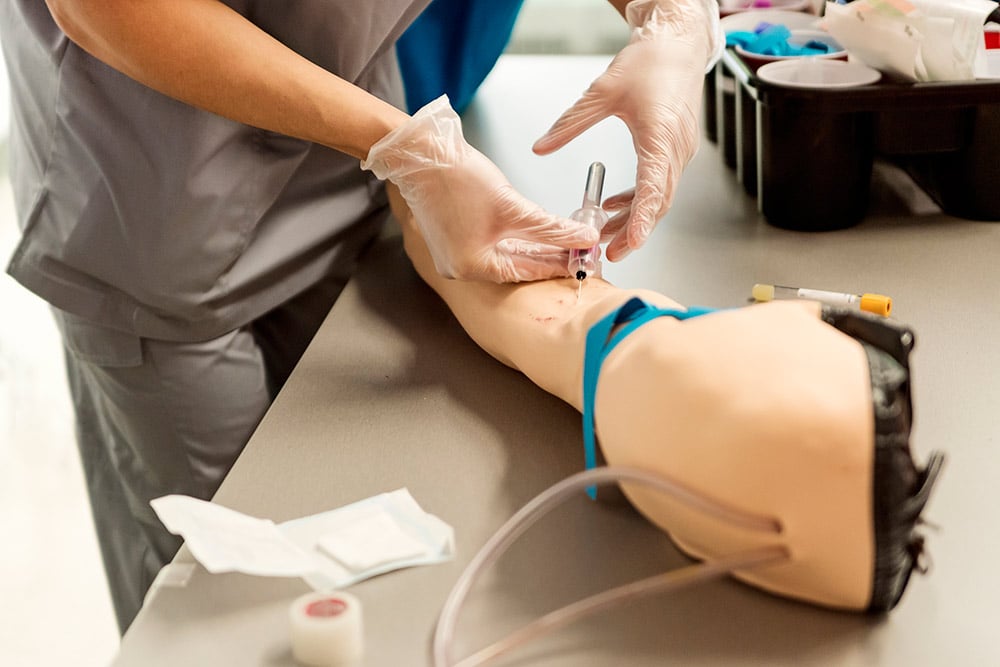
- Students practicing intravenous (IV) insertion techniques on a simulation arm
- Students using an online or paper symptom checker with an image of a human body, which helps students determine possible conditions or illnesses ((SimStaff, “What Is the Difference between Low-Fidelity and High-Fidelity Simulations?”: https://simstaff.com/difference-between-low-fidelity-and-high-fidelity-simulations/))
- Students using written case studies and role-plays with minimal equipment to understand how to properly diagnose and create the best treatment plans ((Government of Western Australia Dept. of Health, “What Is Simulation Learning?” Oct. 10, 2014: https://ww2.health.wa.gov.au/Articles/U_Z/What-is-simulation-learning))
High-Fidelity Simulations for Students
High-fidelity simulations (HFSs) are usually done after LFSs are mastered because they strive to make the simulation as realistic as possible. An HFS might merge an LFS with several other factors that could be present in a real-life scenario. The purpose of an HFS is to test students with a more realistic and complex scenario.
Continuing with the CPR example, once a student masters the chest compressions–to-breath ratio on all three patients (baby, child, and adult), they should be put in an HFS where various realistic possibilities come into play. These possibilities could manifest in the form of environmental changes in the scenario, such as the scene becoming unsafe due to a gas or fire hazard, or due to a highly distressed family member distracting the student. HFS helps prepare students’ technical and situational knowledge, while also giving them practice with handling high-pressure situations.
Other HFS examples include:
- Computer-based manikins that give feedback about drug distribution so students can learn how to inject the correct amount of drugs and identify which ones cannot be used together
- Patients practicing the use of robotic prosthetics, which are controlled by brain activity and thought
- Students using suturing scissors on animal tissue or artificial skin to practice incisions and sutures
Examples of Simulation-Based Learning for Patients

Low-Fidelity Simulations for Patients
Low-fidelity simulations help patients master one small task at a time. LFSs for patients may be analogous to assistive technology devices. Depending on the patient’s injury and prescribed recovery plan, an LFS would test only a couple variables at a time. For instance, if the patient has an eye injury, they could be put in an LFS where the ophthalmologist and their staff test for functionality and movement with an undemanding simulation test.
Examples of LFSs for patients:
- A pediatric nurse may use a walker or rollator to simulate walking independently and helps strengthen kids’ leg muscles.
- Patients can use multisensory devices to simulate the use of the five senses.
- Hand therapy devices assist patients as they practice small movements and also develop range of motion.
High-Fidelity for Patients
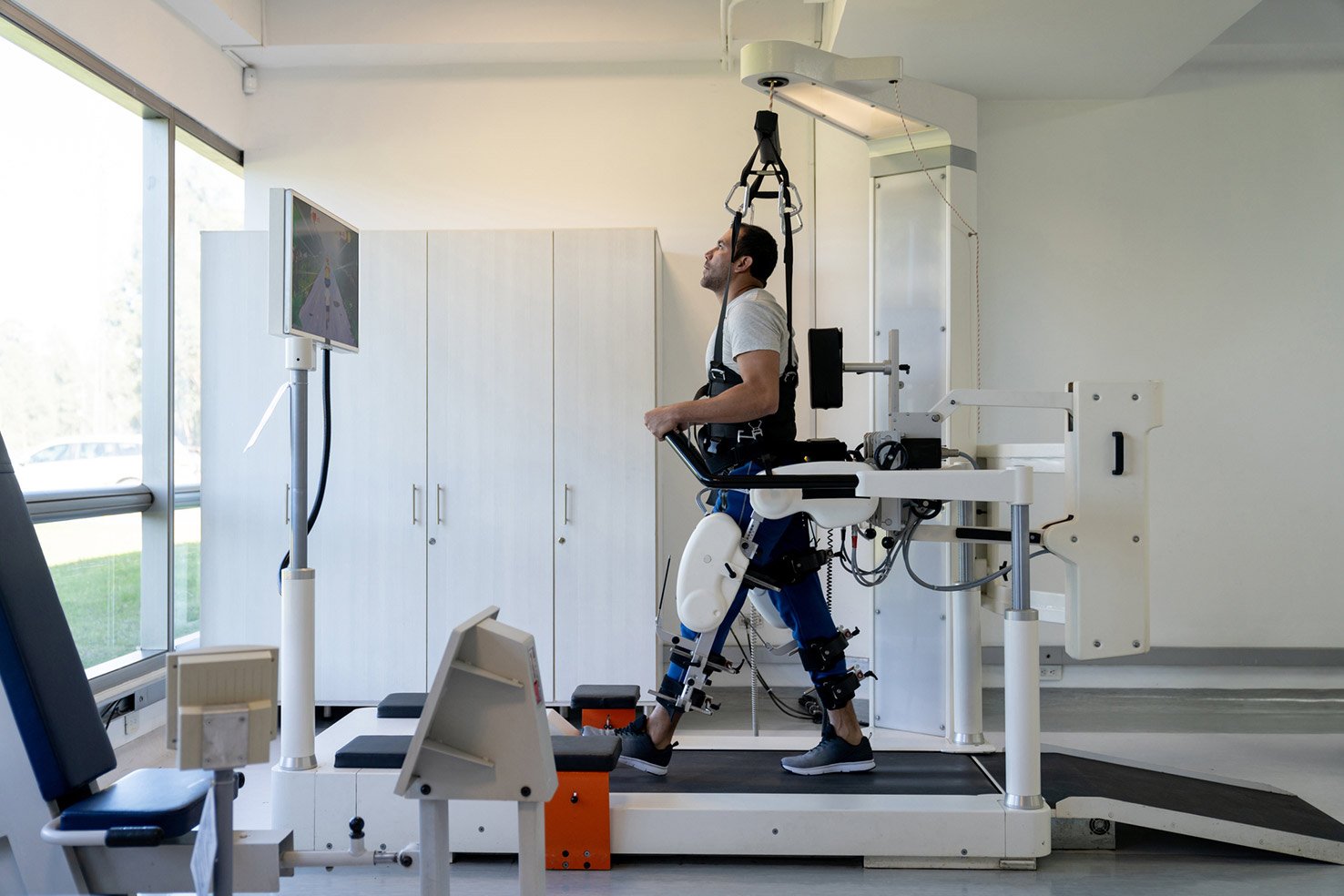
HFSs for patients are used later in treatment after patients have more functionality in the location of impairment or have improved cognition. The purpose of HFSs for patients is to get them in the habit of entering or returning to life with a considerable decrease in assistance from healthcare providers, caretakers, or family members. An example of an HFS is a driving simulation device. These devices are for patients who are close to being able to drive a vehicle but need practice so as not to injure themselves or others.
Another great use of an HFS is to show patients the connections between their physical issues. For instance, a patient might have trouble seeing how their difficulties with preparing food in the kitchen correspond with their inability to drive a vehicle. A good simulation can expose how these difficulties manifest in multiple areas of life and can give the patient and their occupational therapist insight into areas where the patient needs to focus.
Other examples of HFSs for patients include:
- Using a power wheelchair for mobility that is adjusted to suit the patient and their future living space
- Learning to cook with specialized equipment at a rehab facility or in their own home under the guidance of an occupational therapist
- Working with electronic devices to maximize cognition and practice memory retention

The Future of Education Simulation
Technology
Technological advancements are the primary factor in the growth of simulation education. Such advancements are particularly strong in the healthcare field, thanks to the motivation of scientists and physicians to continuously seek out ways they can improve their patients’ lives.
Given the innovative nature of medicine, the healthcare market is a robust candidate for investors and startups looking to build technologies. Already, artificial intelligence (AI) has revolutionized healthcare by improving diagnostics and treatments. Virtual reality offers a way for practitioners such as occupational therapists to experience their patients’ home environments. These and other technologies will continue to impact medical training and education for nurses, occupational therapists, physical therapists, speech-language pathologists, and other healthcare providers.
Assessment
By gathering data on performance, simulations help with the assessment of both student practitioners and patients.
In his article “The Future of Simulation in Medical Education,” Dr. Kieran Walsh predicts, “Performance assessment using simulation will be subject to rigorous evaluation as to its validity, reproducibility, feasibility, acceptability to stakeholders and impact on learning and practice.” This leads us to the need for standardization, or uniformity, within the multitude of simulations put into practice.
Uniformity
Due to the continued need for assessment, it’s key to have uniformity across simulation-based learning. More studies are being conducted to test the validity of simulation-based learning in healthcare programs. ((Caroline Larue, “Simulation in Preparation or Substitution for Clinical Placement: A Systematic Review of the Literature,” Journal of Nursing Education and Practice, July 2015:http://www.sciedupress.com/journal/index.php/jnep/article/view/7069/4432))
As results come in and the effectiveness of different simulations are measured, regularity and consistency across healthcare education will compel some simulations and simulators to be standardized across graduate healthcare programs, while others will become obsolete. However, as technology advances, there will be a back-and-forth between standardizing simulations and using the latest medical and technological advancements. ((Kieran Walsh, “The Future of Simulation in Medical Education,” The Journal of Biomedical Research, May 2015: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4449494/))
Simulations in healthcare education will continue to become more common and uniform across the nation. At USAHS, occupational therapy and physical therapy students participate in a variety of simulations that help them solve puzzles, better communicate with patients, and practice clinical skills. Also, USAHS students from programs such as speech-language pathology, nursing, and others work with one another in simulations to practice how to work in interprofessional healthcare teams.








