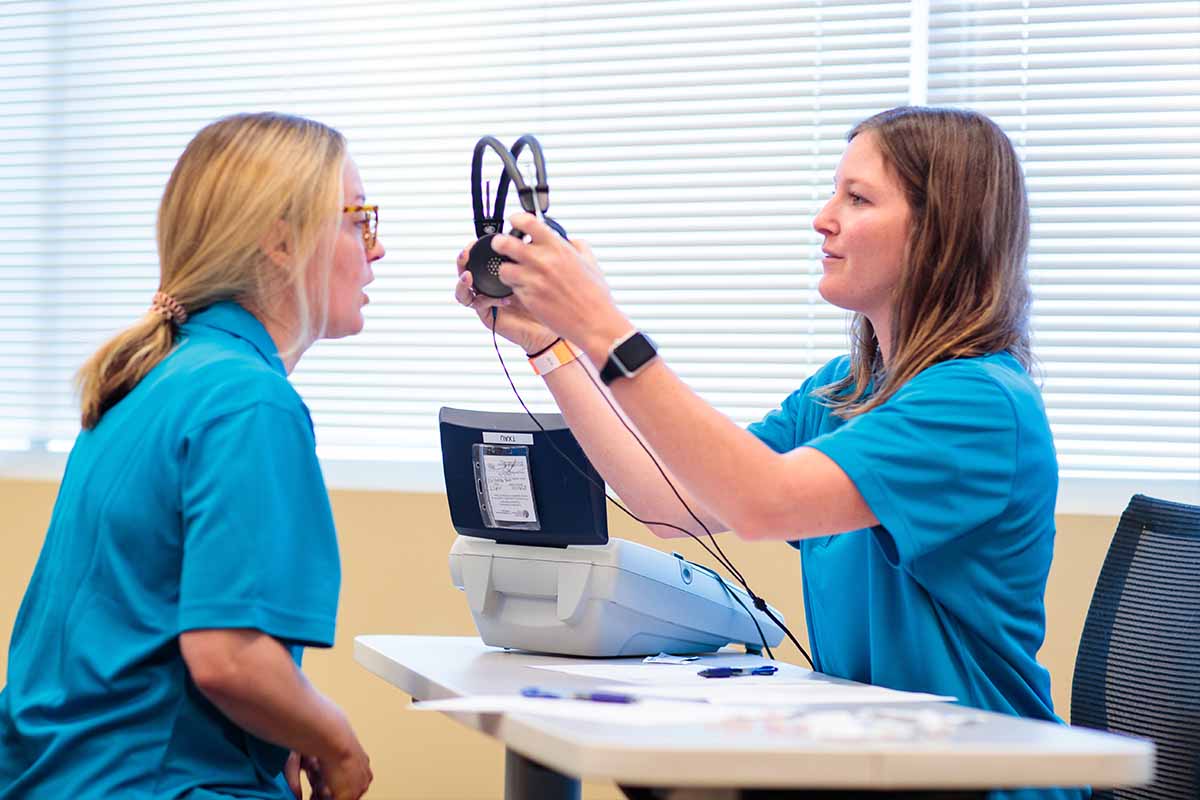
Wanda Baker (R), community health worker, and Nifiah Reid-Sanders, BSN, RN, prepare supplies to administer COVID-19 tests to members of the Detroit community.
Nifiah Reid-Sanders, MSA, BSN, RN, was working as a director in infection prevention and earning her Doctor of Nursing Practice (DNP) degree at USAHS when the first cases of a previously unknown virus began appearing in the United States. It was February 2020. Nifiah and her husband welcomed their daughter and her family to ride out the ensuing pandemic in their home in Ypsilanti, Michigan. First, their grandson came down with pneumonia, possibly contracted at his daycare. Then Nifiah’s husband got sick with a fever of 106°. He was hospitalized and diagnosed with double pneumonia.
At that time, no one realized there was already community spread of COVID-19 in the United States, and testing was not widely available. Much later, her husband’s antibody test would come up positive. Thankfully, both he and their grandson survived. But over the ensuing months, Nifiah lost 12 blood relatives to COVID—two aunts, two uncles, and several first cousins. She also lost several members of her “church family” to the disease.
“All these people were dying all around me,” Nifiah says. “But there were no funerals, no closure. The hardest part was I didn’t know what to do. I felt useless. Previously, I had been part of a lifesaving team in the ICU. Now I was unable to do anything. I was in a dark place for a long time.”
Working Two Roles and Studying During the Pandemic


Nifiah Reid-Sanders, DNP Student at USAHS
Nifiah has been a nurse for nearly 20 years, with eight of those years working in critical care at Michigan Medicine in Ann Arbor. After earning her Master of Health Administration (MHA), she became the Director of Implementation at BioVigil, an infection prevention company. In this role, she travels all over the country and internationally, designing hand hygiene programs for hospitals. She says that although more of her work is virtual now, the company is especially busy “because institutions are more aware, with different protocols in place because of COVID.”
Alongside her work at BioVigil, Nifiah is completing her clinical rotation at Detroit Community Health Connection (DCHC), a non-profit, community-based primary care organization. She has had the opportunity to engage in project management work during this rotation, coordinating and implementing a flu vaccine clinic and now COVID-19 vaccines. She recently completed a pediatric clinical rotation at DCHC as part of earning her Family Nurse Practitioner (FNP) role specialty in the DNP program, and she will sit for the FNP boards this summer.
When she can, she joins the COVID Power Hour, a weekly virtual meeting of USAHS graduate nursing students facilitated by faculty. “We’re all dealing with the same issues,” she says. “Students support one another. You don’t feel like you’re alone.”
Making a Difference in Her Community
But still, despite all her hard work as a director and graduate student, Nifiah felt like she wasn’t doing enough to help people directly impacted by COVID. So, in January 2021, she started volunteering her weekends and some weekdays and has worked with DCHC to provide COVID testing and COVID-19 vaccines to residents throughout the city of Detroit and surrounding areas. She has also partnered with her church, Third New Hope Baptist Church, administering testing and vaccines to members of the congregation and its community. “There’s a historical fear of vaccines in the African-American community,” she says, referring to the U.S. government’s unethical experiments on Black men with syphilis from 1932 to 1972.[1] “That’s a hurdle I’m passionate about overcoming. So, I’m getting out there and educating. I’ve been a member of this church for 22 years. I show a familiar face, one that they trust. I’ve changed a few minds.”
Another hurdle in the city has been vaccine availability; due to issues with distribution, eligibility criteria, and electronic access, Detroit has lagged behind the rest of Michigan in getting its population vaccinated. But healthcare workers are working to address these inequities.
“So many have died around us—people are afraid. Those who are open to the vaccine are super-excited to get that call [for an appointment],” Nifiah says. “I’ve seen people in tears of gratitude.”
Once she passes the FNP board exam, Nifiah plans to continue educating patients about preventive medicine, such as eating healthy and exercising, to keep them out of the ICU.
Now that she is doing something to directly help her community in this pandemic, her grief and sadness have lifted somewhat. “The heart of the nurse is to get in there and do what I can,” Nifiah says. “Now I’m doing that. That’s what’s getting me through this. I always tell people that when I leave, I want to be empty—I want to have given my all.”
The University of St. Augustine for Health Sciences (USAHS) offers a Master of Science in Nursing (MSN) program, a Doctor of Nursing Practice (DNP) program, and Post-Graduate Nursing Certificates designed for working nurses. Our nursing degrees are offered online, with optional on-campus immersions.* Role specialties include Family Nurse Practitioner (FNP), Nurse Educator,** and Nurse Executive. The MSN has several options to accelerate your time to degree completion. Earn your advanced nursing degree while keeping your work and life in balance.
*The FNP role specialty includes two required hands-on clinical intensives as part of the curriculum.
**The Nurse Educator role specialty is not available for the DNP program.
[1] Centers for Disease Control and Prevention, “U.S. Public Health Service Study at Tuskegee”: https://www.cdc.gov/tuskegee/timeline.htm