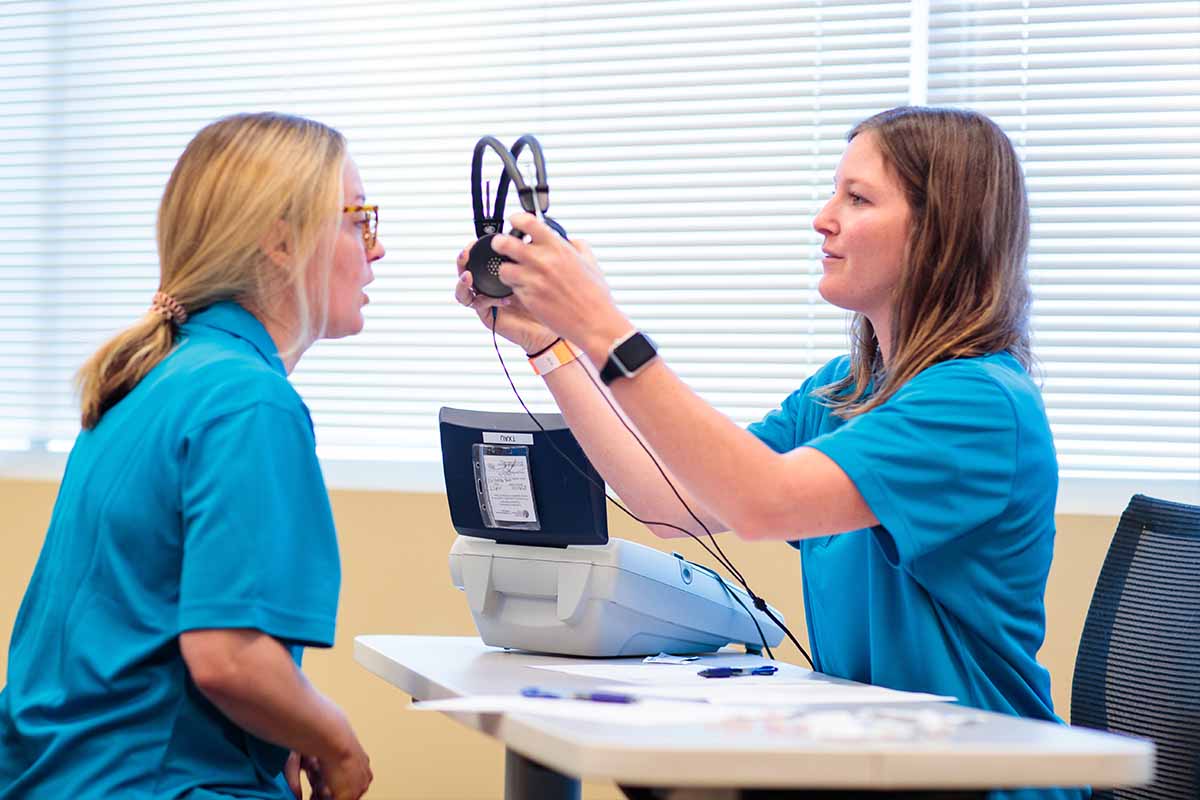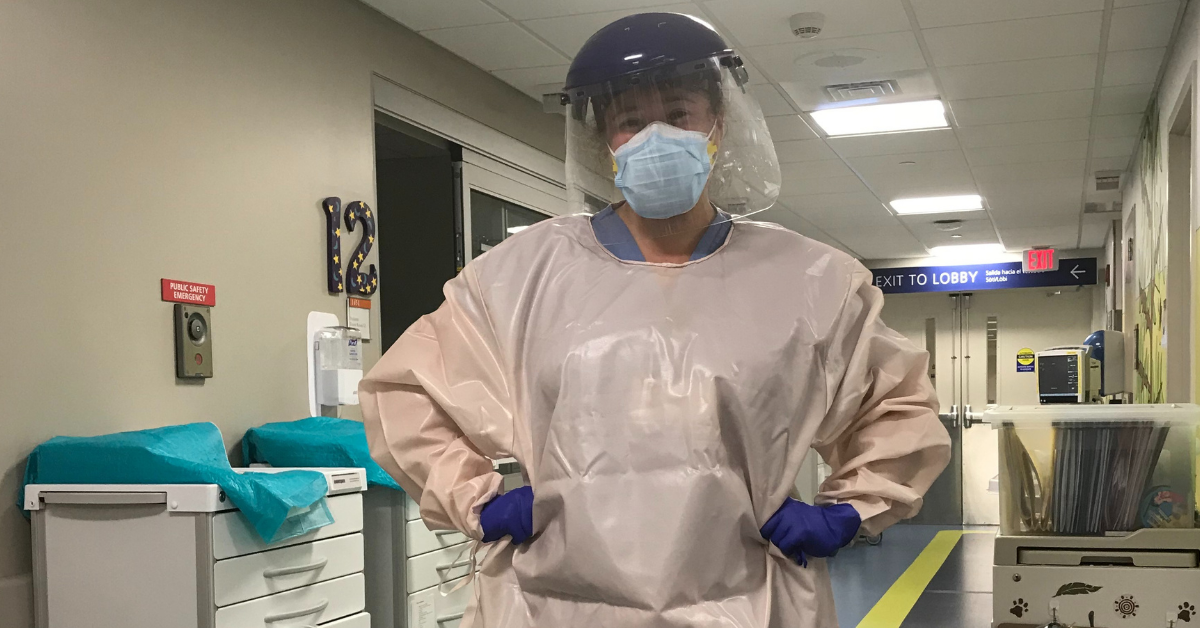
Elizabeth McMaster wearing gown made by Ford Motor Company
When in January 2020 the World Health Organization declared it to be the International Year of the Nurse and Midwife, they didn’t realize how prophetic that was. Within weeks, nurses around the world were working overtime to save patients who were dying of a new, highly transmissible virus. And the public in lockdown cheered our healthcare heroes, banging pots and ringing bells in the streets. Students in USAHS’ graduate nursing programs were among these heroes, working extra shifts in dangerous environments and trying their utmost to save lives.
Riding the First Wave in a Trauma Center
Elizabeth McMaster, BSN, RN, is a student in our Doctor of Nursing Practice program, Nurse Executive specialty. She and her colleagues at a large trauma center in Boston saw what was happening in New York and started planning with the other hospitals in the area. “You’re like a deer in the headlights, seeing this coming,” she says. “We didn’t know how transmissible the virus was, or if our masks would work. But you’re a nurse, and you need to do what you can to help patients.”
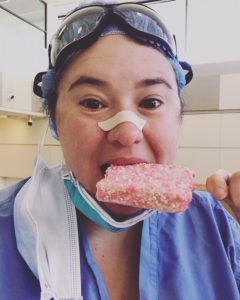

McMaster, DNP student, taking a much-needed break
Soon, COVID patients started to arrive. “The hardest part was not knowing what to expect when someone walked through those doors or when the ambulance arrived,” McMaster says. “Each day, the hospital briefed us on the statistics about patients and staff. We continually learned about better practices and new treatments. Critical thinking was vital to planning patient care. As the number of COVID cases increased, the supply of medications decreased. Medications we’d always taken for granted had to be used efficiently.”
Concerned about the nationwide shortage of personal protective equipment (PPE), McMaster would don all her gear—gown, mask, goggles, face shield, two pairs of gloves—and stay in a patient’s room for up to two hours, using a baby monitor like a walkie-talkie to ask other nurses to retrieve items she needed. Nurses were fortunate to be allocated a new N95 mask each day. At one point, they received gowns made by Ford Motor Company that staff speculated were made from airbag material. “They were reusable and very protective, but also really hot and sweaty,” McMaster says. “They caused your mask and goggles to fog up.”
As cases rose in her area, McMaster often spent nights in hotels to avoid infecting her partner and to reduce her commute time. To reduce cross-contamination, “You change clothes in the car and, once you get home, you take them all off just inside the front door.”
As if all this weren’t stressful enough, her mother, who lives in a nursing home in Philadelphia, contracted COVID early in the pandemic. “I couldn’t do anything for her,” McMaster says. “I wasn’t allowed to visit. I was helping others, but I was not able to help my mom.” Fortunately, her mother survived. But since the start of the pandemic, McMaster has been granted only one hour-long visit to see her mother in person, outside.
Surprising Losses
Heather Josey Thomas, MSN-Ed, RN, CCRN, is a student in USAHS’ DNP program who has been working the front lines of the COVID pandemic in two hospitals in Augusta, Georgia. Although she is accustomed to stress as a single mom and longtime ICU nurse, Thomas says the peak of the pandemic brought new levels of stress—and a lot of loss.
“We can usually tell whether someone will make it out of ICU just based on mortality predictors and co-morbidities when they come in,” Thomas says. “During COVID, we would get patients in who were thirty to forty years old and healthy-looking, and they would die anyway. Their turn for the worse came suddenly, and too many times we couldn’t pull them back. The loss was tough because it took us by surprise.”
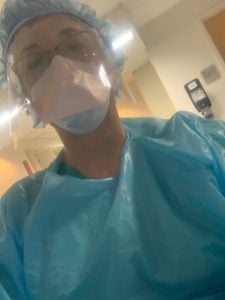

Heather Thomas, DNP student, in full PPE
“There have been patients who we thought would make it,” she continues. “We got them off life support and discharged home—only to have them come back and die from long COVID. We’ve had some very frail, elderly folks come in for another problem, only to find out they are COVID-positive and have no symptoms at all. So the whole thing has been an emotional rollercoaster ride. Setting up video chat for families to say goodbye to a loved one they can’t ever hug again is hard. Watching them cry on an iPad as their person slips away puts a lump in my throat, even now.”
Getting Through It
A few things kept McMaster going through the worst of the pandemic. Her boyfriend and family were a source of support, and public recognition of healthcare workers buoyed her. Restaurants sent free lunches; the hospital rewarded frontline nurses with overtime and bonus pay. “You had to do it, so you do it,” she says. “There’s a camaraderie in doing it together. You learn to trust your team members. Everyone got closer.”
Of course, McMaster was not only working long hours—she was also earning her DNP. She credits faculty member Amy Herrington, DNP, RN, CEN, with helping her cope. “She checked up on me at least once a week,” McMaster says. There was also the COVID Power Hour, a support group for USAHS nursing students that Dr. Herrington co-founded. “You share what you’re going through,” says McMaster. “It’s a source of education and information.” From the relationships made in this group, nurses in California sent PPE to nurses in areas that were harder-hit earlier in the pandemic. A psychiatric nurse practitioner called “Dr. Jenn” provided emotional support, advice, and techniques for meditation and self-care.
Thomas also praises this initiative. “The COVID Power Hour was instrumental for me in maintaining my sanity. Just being able to get on there and hear how my peers in other states were doing, what things they were trying, and what successes or failures they were experiencing was immensely helpful.”
Shifting Hospital Personnel
In August 2020, McMaster transitioned to a new role as nurse manager. As of May 2021, she is a director at the hospital. “To become a nurse executive was a reason I went back to school,” she said. “Earning my DNP made me a strong candidate for this position.” Although McMaster had previous experience in management, she found it challenging to assume this role in the middle of COVID, as the pandemic had significantly impacted hospital finances. Elective surgeries had shut down—a main source of revenue—and with other patients staying away out of fear of infection, staffing had to be shifted. McMaster was part of some of these difficult staffing decisions. “It’s hard for people to handle change when they’re already so stressed,” she says.
Thomas reports similar situations at the two hospitals where she works. One hospital mandated overtime and reallocated staff to cover COVID units. “Detailed staff may have worked in say, an outpatient clinic and then found themselves in med-surg floor nursing roles,” she says. “Nurse anesthetists found themselves back at the ICU bedside, even if they had not been direct care nurses in decades.” Her other hospital hired traveling and agency nurses to fill the gaps. “They offered a huge COVID differential, essentially doubling everyone’s hourly salary—but eventually, even that couldn’t entice people to work extra shifts because we were just so tired.”
The Light at the End of the Tunnel
Now, more than one year since the pandemic began, McMaster’s hospital is “completely on top of it.” Not only have staff figured out COVID treatment protocols that are saving lives—they have also created positive new social services initiatives, including a food bank, mobile healthcare for the homebound, and a bridge psychiatric clinic to address the increase in behavioral health issues during the pandemic. They have expanded the use of telemedicine and are making follow-up phone calls to check on our COVID patients. “A lot of good things have come from this.”
McMaster has words of advice for other nurses who are earning their graduate degree. “You don’t know how far you can push yourself until you do it. If you can go through the program while working during a pandemic, and do well—what else can you accomplish in life? If I hadn’t done this, I wouldn’t know what I was capable of.”
The University of St. Augustine for Health Sciences (USAHS) offers a Master of Science in Nursing (MSN) program, a Doctor of Nursing Practice (DNP) program, and Post-Graduate Nursing Certificates designed for working nurses. Our nursing degrees are offered online, with optional on-campus immersions* (currently postponed due to COVID-19). Role specialties include Family Nurse Practitioner (FNP), Nurse Educator,** and Nurse Executive. The MSN has several options to accelerate your time to degree completion, allowing you to complete coursework when you want and earn your advanced nursing degree while keeping your work and life in balance.
*The FNP role specialty includes two required hands-on clinical intensives as part of the curriculum.
**The Nurse Educator role specialty is not available for the DNP program.