Have you ever wondered, “What is pelvic floor therapy?” You are not alone. Pelvic floor physical therapy is a specialized area of physical therapy (PT) that focuses on improving bladder and bowel control, sexual function and stability by addressing the muscles, connective tissue and coordination of the pelvic floor.1
Often referred to as pelvic floor PT, this advanced practice requires training beyond a standard Doctor of Physical Therapy (DPT) program. Pelvic health physical therapists (PTs) pursue additional specialized education and hands-on training to effectively evaluate and treat complex pelvic health conditions across the lifespan.1
- The DPT program at the University of St. Augustine for Health Sciences (USAHS) provides foundational skills for graduates who may decide to pursue pelvic floor pt specialization.
Pelvic floor physical therapy is a specialty within physical therapy focused on the muscles, connective tissue and nerves of the pelvis. These structures are essential for bladder and bowel control, support of reproductive organs, sexual function and core stability. Pelvic health PTs evaluate how these muscles and systems are working and design treatments to improve overall function.1,2
At USAHS, we prepare physical therapists to build a strong foundation for specialty practice, including pelvic floor therapy. Let’s review who may benefit from pelvic floor PT, what research says about its effectiveness and how our physical therapy programs can help you prepare to pursue this focused area of care.
Pelvic Floor Basics: Muscles, Function and Common Problems
The pelvic floor is a complex network of muscles and ligaments located at the base of the pelvis. It supports the bladder, uterus, prostate and more. Together, the structures of the pelvic floor contribute to continence and sexual function, and even play a role in core stability.3
Pelvic floor dysfunction occurs when the muscles or supporting structures are weak. Common problems include urinary or fecal incontinence, pelvic organ prolapse, chronic pelvic pain, sexual dysfunction and difficulty with bowel or bladder emptying.
Pelvic Floor Disorders
According to the Pelvic Floor Disorders Network (PFDN) and the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), pelvic floor disorders (PFDs) include urinary incontinence, fecal incontinence, pelvic organ prolapse and other abnormalities of the lower urinary and gastrointestinal tracts.4,5
Pelvic floor symptoms can begin during pregnancy, with about 50% of pregnant women experiencing signs of pelvic floor disorders even before childbirth. 6 PFDs are more common in women.7 However, men can also experience pelvic floor dysfunction, related to chronic constipation or pelvic pain.2 These issues can make it difficult for women to lead comfortable lives.
What Are Pelvic Floor Physical Therapists?
Pelvic floor physical therapists are licensed physical therapists who have training in evaluating and treating pelvic floor muscle dysfunction. These practitioners are movement experts who receive specialized postgraduate education and clinical training to safely perform internal and external pelvic assessments and deliver interventions tailored to the pelvic region.1
Pelvic health PTs:
- Assess muscle strength, coordination and flexibility
- Design individualized exercises to restore function
- Teach relaxation techniques for tight or overactive muscles
- Address symptoms like incontinence, prolapse, pelvic pain or bowel dysfunction
Their goal is to improve quality of life by restoring pelvic health and supporting participation in work, recreation and family life that patients may struggle with. Pelvic floor PT during pregnancy and postpartum pelvic floor physical therapy are two examples of specialized pelvic health care that support people through major body changes and help address common concerns like pain, incontinence and core or pelvic stability.
How to Become a Pelvic Floor Therapist
If you are interested in becoming a physical therapist who helps patients who suffer from PFDs, there’s a clear course of work you’ll need to complete. USAHS offers graduate physical therapy programs that can prepare you to pursue this career.
Doctor of Physical Therapy (DPT)
To become a licensed physical therapist in the U.S., you must earn a Doctor of Physical Therapy (DPT) degree from a Commission on Accreditation in Physical Therapy Education (CAPTE)-accredited program and pass a state licensure exam.8,9
At USAHS, our DPT program offers innovative and outcome-focused learning through immersive coursework and hands-on labs that build foundational skills in musculoskeletal, neurologic and cardiopulmonary care. While specialization in pelvic health occurs after licensure, USAHS graduates are well-prepared for advanced training through a combination of evidence-informed practice, anatomy education and patient-centered care.
NPTE and State Licensure
After completing a CAPTE-accredited DPT program, like the DPT program at USAHS, candidates must pass the National Physical Therapy Examination (NPTE) to obtain licensure. State boards may have additional requirements, but passing the NPTE is essential for practicing as a physical therapist in any U.S. state.10
Develop Clinical Experience as a Practicing PT
Before specializing in pelvic health, many physical therapists spend time practicing as general PTs to strengthen their core clinical skills. Working with patients in settings such as hospitals, outpatient clinics or rehabilitation centers helps therapists build experience in evaluation, treatment planning and patient care across a range of conditions.11
Pursue Pelvic Health-Specific Continuing Education
Specialized pelvic floor training for physical therapists is considered continuing education. APTA Pelvic Health offers structured courses that cover internal pelvic exams, pelvic pain, bowel dysfunction, pregnancy and postpartum care and patient populations with unique needs.11
These courses are typically taken after licensure and can include Level 1-3 training, mentorship opportunities and clinical practice experience, allowing therapists to develop the advanced skills needed for pelvic health care.


How USAHS Prepares PTs Who May Specialize in Pelvic Health
At USAHS, we prepare physical therapists for long-term growth and post-graduate specialization by building a strong clinical foundation through our DPT curriculum.
As a student, you’ll develop:
- A solid base in anatomy, physiology and biomechanics. You’ll learn how muscles, nerves and joints work together, knowledge that supports effective evaluation and treatment across body systems, including the pelvic floor.
- Evidence-informed assessment and treatment skills. We emphasize using research to guide clinical decision-making so your interventions are safe, effective and responsive to each patient’s presentation.
- Patient-centered clinical reasoning. You’ll learn to look at the whole person, including goals, lifestyles and daily demands, then translate that into plans of care that support function and quality of life.
- Hands-on practice through labs and immersive clinical education. You’ll train in supervised, realistic environments that help you build confidence and competence before stepping into real-world clinical settings.
Together, these skills can help you pursue advanced training in pelvic health after graduation, so you’re prepared to treat patients with pelvic floor dysfunction across the lifespan, supporting diverse needs and diagnoses.
Your Career in Pelvic Floor Physical Therapy
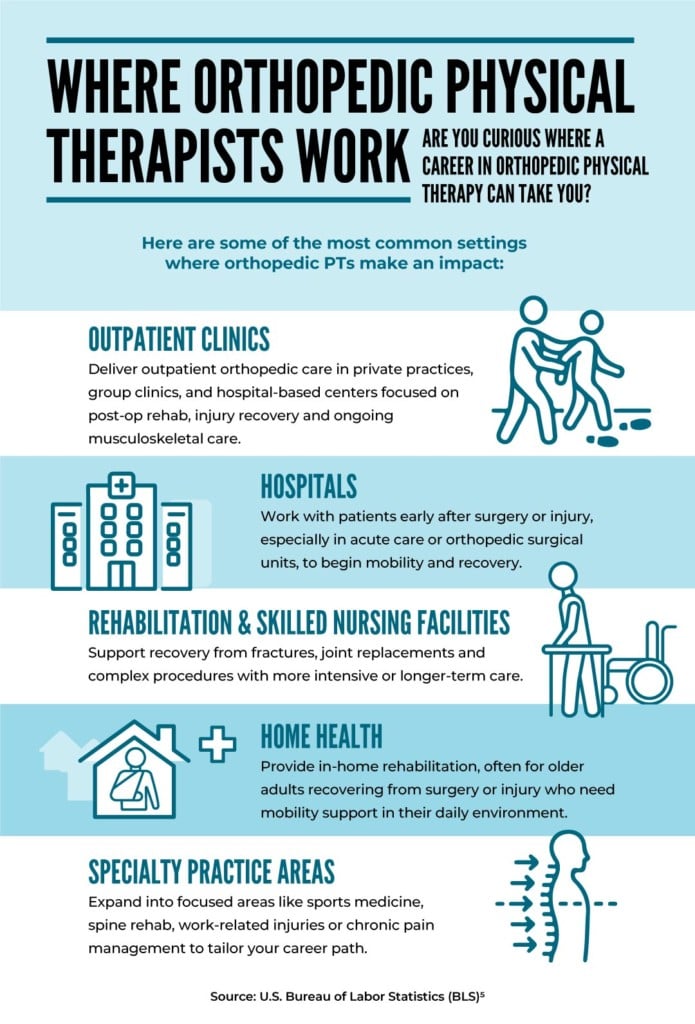
Demand for physical therapists continues to grow, and as pelvic health becomes a bigger part of mainstream care, the need for PTs with pelvic health expertise increases as well. As a pelvic health physical therapist, you may work in outpatient clinics, hospitals, rehabilitation centers or private practices.12
In this specialty, you can support patients across the lifespan, from prenatal and postpartum individuals to older adults managing pelvic organ prolapse or incontinence. Your work addresses pelvic floor dysfunction so patients can move with confidence, improve daily function and protect their independence and quality of life.
This career is rewarding, and with hard work and a commitment to success, you can achieve it. USAHS is here to help guide you toward a rewarding pelvic floor physical therapy career.


FAQs
What is pelvic floor therapy?
Pelvic floor therapy is a branch of physical therapy that focuses on the muscles, ligaments and connective tissue of the pelvis. It aims to improve bladder and bowel control, relieve pelvic pain, support sexual function and strengthen core stability.1,2
Treatment may involve guided exercises, manual therapy, biofeedback and education on posture and movement patterns to reduce strain on the pelvic floor.1,2
How is pelvic floor therapy different from physical therapy?
While all physical therapists are trained in movement, musculoskeletal and functional rehabilitation, pelvic floor physical therapists complete additional specialized education to safely assess and treat internal and external pelvic structures.1
They focus on issues that directly affect the pelvis, such as incontinence, prolapse, pelvic pain and bowel dysfunction.
References:
- “Benefits of Pelvic Health Physical Therapy,” APTA Pelvic Health, An Academy of the American Physical Therapy Association (APTA), July 6, 2024, https://www.aptapelvichealth.org/info/the-benefits-of-pelvic-health-physical-therapy.
- “Overview: Pelvic Floor Disorders,” Northwestern Medicine, 2026, https://www.nm.org/conditions-and-care-areas/womens-health/obgyn/pelvic-health/pelvic-floor-disorders.
- “Pelvic Floor Muscles: Anatomy, Function & Conditions,” Cleveland Clinic, June 27, 2025, https://my.clevelandclinic.org/health/body/22729-pelvic-floor-muscles.
- “Pelvic Floor Disorders Network (PFDN),” Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) May 22, 2024, https://www.nichd.nih.gov/research/supported/pelvicfloor.
- “NICHD Pelvic Floor Disorders (PFDs) Research Information,” Eunice Kennedy Shriver National Institute of Child Health and Human Development (NIHCD), May 22, 2024, https://www.nichd.nih.gov/health/topics/pelvicfloor/researchinfo.
- Khalife, T., “Pregnancy’s Effect on Pelvic Floor Health,” Mayo Clinic Health System, May 23, 2023, https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/pregnancys-effect-on-pelvic-floor-health.
- Pelvic Floor Disorders Network, https://pelvicfloordisordersnetwork.org/.
- “Becoming a Physical Therapist,” American Physical Therapy Association (APTA), . https://www.apta.org/your-career/careers-in-physical-therapy/becoming-a-pt.
- Commission on Accreditation in Physical Therapy Education (CAPTE), https://www.capteonline.org/.
- “National Exam (NPTE®),”Federation of State Boards of Physical Therapy (FSPBT), https://www.fsbpt.org/Secondary-Pages/Exam-Candidates/National-Exam-NPTE.
- APTA Pelvic Health, An Academy of the American Physical Therapy Association (APTA), ” https://www.aptapelvichealth.org/.
- “Become a Pelvic Health Physical Therapist (PT),” APTA Pelvic Health, An Academy of the American Physical Therapy Association (APTA), November 10, 2023, https://www.aptapelvichealth.org/info/become-a-pelvic-health-physical-therapist-pt.